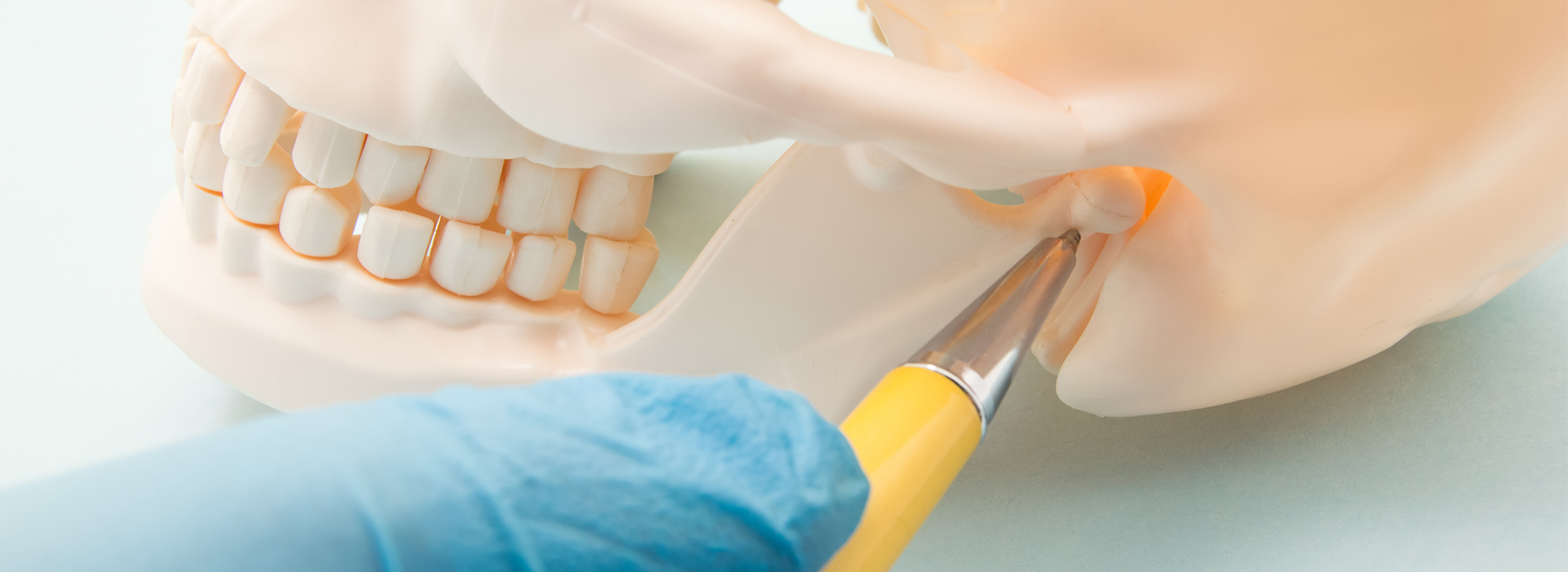
The temporomandibular joints (TMJs) connect the lower jaw to the skull on both sides of the face and coordinate a surprising range of movement. Unlike a simple hinge, each joint combines hinge and sliding actions to let you open and close your mouth, move the jaw side to side, and push it forward and back. A small, fibrous disc sits between the jawbone and the temporal bone to cushion and guide those movements.
Because the TMJ works with muscles, ligaments and dental surfaces all at once, disturbances in any of these parts can affect how the joint functions. Even small shifts in tooth contact or repetitive muscle tension can change the way forces travel through the joint, leading to discomfort or altered motion. That complexity is why TMJ problems are often experienced as a cluster of symptoms rather than a single, obvious sign.
Understanding the anatomy and mechanics of the joint helps explain why diagnosis and care take a measured approach. The goal is to restore natural movement and comfort while addressing any contributing factors—muscular, skeletal or dental—so that everyday activities like chewing, speaking and yawning feel normal again.
TMJ disorders most often arise from a combination of mechanical strain and biological vulnerability. Frequent teeth grinding (bruxism) or clenching places sustained pressure on the joints and surrounding muscles, gradually producing soreness, inflammation and changes in the disc position. Acute jaw injuries—whether from a fall, a sports impact or a heavy blow—can also trigger immediate joint dysfunction.
Arthritic conditions, such as osteoarthritis or rheumatoid arthritis, may produce degenerative changes inside the joint that alter its shape and smooth function. In addition, habitual behaviors like prolonged gum chewing, biting nails, or resting the jaw on a hand can create repetitive strain. Stress and sleep disturbances also contribute by increasing parafunctional muscle activity, so psychological and lifestyle factors are frequently relevant.
Dental alignment and bite relationships play a role as well. When the way upper and lower teeth meet is uneven, the jaw may shift to find a comfortable position, increasing load on particular parts of the joint. That’s why a complete evaluation looks beyond the joint itself to include muscle function, dental contacts and overall posture.
TMJ disorders can present in many ways, and symptoms often overlap with other conditions. Common complaints include jaw pain or tenderness, difficulty opening the mouth fully, and audible clicking, popping or grating sounds during movement. Some people notice the jaw temporarily “locking” in an open or closed position, or a limited range of motion that makes chewing uncomfortable.
Pain associated with TMJ dysfunction frequently radiates beyond the joint. Headaches concentrated at the temples, ear pain or fullness, a ringing sensation (tinnitus), and neck or upper-back discomfort may all be connected to jaw mechanics. Because these symptoms can resemble ear or sinus problems, a dental evaluation can be important when typical medical causes have been ruled out.
It’s also common for symptoms to fluctuate—worsening during periods of stress, after dental work, or following a night of clenching. Even if pain is intermittent or relatively mild, persistent functional changes (like difficulty chewing or consistent jaw noises) are reason enough to seek a professional assessment so issues can be addressed before they progress.
An accurate diagnosis begins with a thorough clinical exam that assesses jaw movement, joint sounds, muscle tenderness and how the teeth come together. Dental professionals look for asymmetry in motion, limitations in opening, and reproducible pain provoked by specific movements. This hands-on assessment helps narrow the likely sources of a patient’s symptoms.
When additional information is needed, imaging can reveal structural details. Panoramic X-rays, magnetic resonance imaging (MRI) and cone beam computed tomography (CBCT) each contribute different insights—soft-tissue position, disc condition and bony anatomy, respectively. A careful diagnostic approach combines clinical findings with targeted imaging only when it will meaningfully influence treatment decisions.
Because TMJ disorders can reflect muscle, joint or dental origins—or a mix of all three—many evaluations involve input across disciplines. Dentists experienced in occlusion and jaw pain may coordinate with physical therapists, otolaryngologists or rheumatologists when symptoms suggest systemic disease or when conservative measures require reinforcement.
Treatment typically begins conservatively. Self-care measures—such as adopting a soft-food diet temporarily, avoiding extreme jaw movements, applying heat or cold and practicing relaxation techniques—often reduce muscle tension and improve comfort. Simple behavioral changes that limit clenching and jaw-loading can make a meaningful difference over weeks.
Occlusal appliances, like custom night guards, are commonly used to reduce the effects of bruxism and to protect tooth surfaces while the muscles settle. Physical therapy that focuses on stretching, posture correction and neuromuscular retraining may improve coordination and decrease painful muscle activity. In many cases, these noninvasive strategies restore function without the need for more aggressive intervention.
When symptoms persist despite conservative care, clinicians may consider targeted therapies such as medication for inflammation or muscle spasm, corticosteroid injections for localized joint inflammation, or botulinum toxin in select cases to reduce severe muscle hyperactivity. Surgical procedures are reserved for structural joint problems that do not respond to other treatments; these are discussed only after careful evaluation and when clear objective findings justify intervention.
Because TMJ disorders often involve more than one factor, the most successful plans are customized and may combine home care, oral appliances, physical therapy and, when needed, medical or dental procedures. A measured, stepwise approach prioritizes the least invasive options first and tailors escalation only to individual needs and diagnostic findings.
Summary: If recurring jaw pain, clicking, limited opening or related headaches are affecting daily life, a focused evaluation can identify contributing factors and outline a personalized plan for relief. The team at A Plus Dentistry combines clinical examination with appropriate imaging and collaborative care to diagnose TMJ disorders accurately and recommend treatments that prioritize function and comfort. If you have questions or would like to discuss your symptoms, please contact us for more information.
The temporomandibular joints (TMJs) connect the lower jaw to the skull and allow complex hinge and sliding movements needed for chewing, speaking and yawning. A TMJ disorder describes a group of conditions that affect the joint, the cushioning disc, the surrounding muscles or the way the teeth meet. Symptoms can include muscle soreness, joint noises, limited range of motion and pain that radiates to the head, neck or ears. Because several structures work together to produce normal jaw function, TMJ disorders often present as a cluster of signs rather than a single clear symptom.
Some problems result from soft-tissue issues such as muscle tension or disc displacement, while others arise from degenerative changes in the joint surfaces or trauma. Identifying which structures are involved is essential to creating a tailored plan that restores comfortable, natural movement. Clinicians prioritize conservative, reversible therapies when possible to preserve function and minimize risk. Early assessment helps prevent chronic pain patterns and improves the chance that simple measures will be effective.
Common symptoms that deserve a dental evaluation include persistent jaw pain or tenderness, clicking, popping or grating noises during movement, and episodes of the jaw locking open or closed. Difficulty opening the mouth fully or a restricted range of motion that interferes with chewing are also important signs. Pain that radiates to the temples, ears or neck and headaches linked to jaw activity should prompt assessment because they can be related to TMJ dysfunction. Even intermittent symptoms that affect daily function or sleep warrant attention to catch issues before they become chronic.
If you notice rapid tooth wear, morning soreness in the jaw muscles, or consistent changes in your bite, scheduling an evaluation can clarify the cause. A dental exam helps distinguish TMJ-related problems from ear, sinus or neurological causes and directs appropriate testing when needed. Keeping a simple symptom diary noting triggers and timing—such as stress, dental work or specific activities—can provide useful diagnostic clues. Early diagnosis increases the likelihood that noninvasive care will relieve symptoms.
TMJ disorders usually arise from a combination of mechanical strain and individual vulnerability rather than a single cause. Frequent clenching or grinding of the teeth (bruxism) places sustained pressure on the joint and surrounding muscles, which can lead to soreness, inflammation and changes in disc position. Acute trauma to the jaw from accidents or impacts can also trigger joint dysfunction, while repetitive habits such as prolonged gum chewing or resting the jaw on a hand create ongoing strain. Stress and sleep disturbances commonly increase parafunctional muscle activity and are frequent contributors.
Arthritic conditions like osteoarthritis or rheumatoid arthritis may produce degenerative changes that affect joint shape and smooth motion, and dental alignment can influence how forces are distributed across the TMJ. When upper and lower teeth meet unevenly, the jaw may shift to find a comfortable position, increasing load on particular joint areas. Because many factors interact, a comprehensive evaluation reviews muscle function, joint mechanics, dental contacts and broader postural or systemic issues. Treatment is most effective when it addresses the specific combination of contributing factors for each patient.
Diagnosis begins with a detailed clinical exam that evaluates jaw movement, joint sounds, muscle tenderness and how the teeth come together. Clinicians assess range of motion, observe asymmetry in movement, listen for reproducible clicks or crepitus and palpate muscles and joints to identify sources of pain. A careful evaluation of dental contacts and bite relationships is included because occlusion can influence joint loading. This hands-on assessment narrows the likely causes and guides whether additional testing is necessary.
When imaging will influence treatment decisions, dentists may order panoramic X-rays, magnetic resonance imaging (MRI) or cone beam computed tomography (CBCT) to visualize soft-tissue position, disc condition and bony anatomy respectively. MRI is particularly useful for assessing disc displacement and soft-tissue pathology, while CBCT provides detailed information about the bone. Multidisciplinary input from physical therapists, otolaryngologists or rheumatologists can be valuable when symptoms suggest systemic disease or when conservative measures need reinforcement. The diagnostic plan is individualized so that tests are used purposefully to inform care.
Simple self-care often reduces muscle tension and improves comfort. Adopting a soft-food diet temporarily, avoiding extreme jaw movements such as wide yawning or biting into hard foods, and limiting gum chewing can decrease direct joint loading. Applying moist heat or cold packs to the jaw area and practicing relaxation techniques like diaphragmatic breathing or progressive muscle relaxation can lower parafunctional muscle activity. Improving sleep hygiene and managing stress are important because nighttime clenching frequently worsens symptoms.
Gentle, guided jaw exercises and stretches recommended by a clinician or physical therapist can restore range of motion and promote coordinated muscle activity. Mindful awareness of jaw posture—keeping teeth slightly apart and lips together when not chewing—helps reduce chronic clenching. While many patients see improvement over several weeks with consistent self-care, keeping a record of symptom triggers and response to measures helps clinicians refine the treatment plan. If symptoms persist or worsen, seek professional evaluation for targeted therapies.
Custom occlusal appliances and night guards are commonly used to reduce the damaging effects of bruxism and to allow the muscles and joint to relax. These devices provide a protective barrier for tooth surfaces, distribute biting forces more evenly and can temporarily alter jaw position to reduce joint strain. Because they are fabricated to fit the patient precisely, custom appliances are more comfortable and effective than over-the-counter alternatives. Many clinicians also use trial appliance therapy diagnostically to determine whether splint-based treatment improves symptoms.
Appliances are rarely a standalone cure but can be an important part of a stepwise plan that includes behavior modification and physical therapy. Regular follow-up is necessary to adjust the appliance as symptoms change and to prevent adverse effects from an improperly fitted device. In some cases the appliance reduces muscle hyperactivity and tooth wear but additional interventions are required to address underlying causes. The goal is to use the appliance as a reversible, conservative therapy while assessing longer-term strategies if needed.
Physical therapy targets the muscular and postural contributors to TMJ pain through stretching, strengthening, manual therapy and neuromuscular re-education. Therapists teach targeted exercises to improve jaw coordination, shoulder-neck posture and breathing patterns that influence muscle tension. Soft-tissue techniques, joint mobilization and home exercise programs often reduce pain and restore function when combined with other conservative measures. Physical therapy can be particularly helpful for patients whose symptoms are closely linked to postural strain or muscular imbalance.
Because TMJ disorders can involve dental, musculoskeletal and systemic factors, multidisciplinary collaboration often yields the best outcomes. Dentists, physical therapists, otolaryngologists and rheumatologists may coordinate care when symptoms suggest joint degeneration, systemic inflammation or overlapping ENT issues. This team approach ensures that interventions are complementary and that invasive procedures are considered only after conservative options have been optimized. Clear communication among providers helps tailor a long-term plan focused on function and comfort.
Advanced interventions such as corticosteroid injections, botulinum toxin or surgical procedures are generally considered only after conservative treatments have been tried and when diagnostic findings support their use. Corticosteroid injections can reduce localized joint inflammation in select cases, while botulinum toxin may be used judiciously to reduce severe muscle hyperactivity that does not respond to other therapies. These options carry specific risks and benefits that clinicians review carefully with patients and are chosen based on clinical examination and imaging. Decision-making emphasizes minimally invasive steps first and reserves more invasive measures for clearly indicated structural problems or refractory pain.
Surgical procedures range from arthrocentesis and arthroscopy to open joint reconstruction and are typically pursued only for persistent mechanical problems or advanced degenerative disease documented on imaging. Preoperative planning often involves specialists and may include pain management, rheumatology or maxillofacial surgery consultations. Because outcomes depend on proper patient selection and technique, surgery is a measured option after exhaustive conservative care. Follow-up rehabilitation and long-term monitoring are important parts of any advanced treatment pathway.
Dental treatments such as orthodontics or restorative procedures can sometimes change how the teeth meet and thereby alter joint loading, which may help selected patients with TMJ-related symptoms. When bite relationships contribute to dysfunction, coordinated dental care that carefully evaluates occlusion can be beneficial as part of a comprehensive plan. However, irreversible or aggressive occlusal changes should be approached with caution because altering tooth position or vertical dimension without clear evidence can create new problems. Treatments that change the bite are considered only after a thorough diagnostic workup and when the expected benefits outweigh the risks.
Conservative, reversible approaches are preferred initially to determine whether symptoms respond to noninvasive measures. If long-term occlusal modification is contemplated, clinicians commonly involve interdisciplinary input and use reversible testing methods first, such as provisional restorations or diagnostic appliances. Ongoing monitoring ensures that dental interventions are supporting improved function rather than perpetuating pain. Patient education and shared decision-making guide the choice and timing of any restorative or orthodontic plan aimed at addressing TMJ issues.
The practice begins with a focused clinical examination that reviews jaw movement, joint sounds, muscle tenderness and dental contacts to identify likely contributing factors. When indicated, targeted imaging such as panoramic X-rays, CBCT or MRI is used to clarify soft-tissue or bony findings and to guide treatment selection. Care typically follows a stepwise approach that emphasizes self-care, occlusal appliances, and physical therapy, with progression to medical or procedural options only if conservative measures fail. Treatment plans are individualized and may involve coordination with physical therapists or medical specialists as needed.
Education and gradual progression of therapy are central to the practice philosophy so patients understand the rationale for each step and expected outcomes. If symptoms are affecting daily life, a focused evaluation at our Cumming, Georgia office can identify contributing factors and outline a personalized plan for relief. The goal is to restore comfortable, natural jaw movement while minimizing invasive interventions and prioritizing long-term function. Patients are encouraged to schedule an assessment to discuss their specific symptoms and treatment options.
Quick Links