Millions of people feel uneasy about dental visits — from mild nerves to full-blown dental phobia. If anxiety has kept you from getting the care you need, sedation dentistry can change that. Our team at A Plus Dentistry provides thoughtful, evidence-informed sedation options that help patients stay relaxed and receive comprehensive dental treatment without unnecessary stress.
Rather than glossing over fear, modern sedation practices acknowledge it and offer carefully controlled methods to manage it. Sedation can make routine cleanings and complex procedures alike more comfortable, shorten appointment-related distress, and improve the likelihood that patients will follow through with recommended care. Below, you’ll find clear explanations of how sedation works, who benefits most, and what to expect before, during, and after treatment.
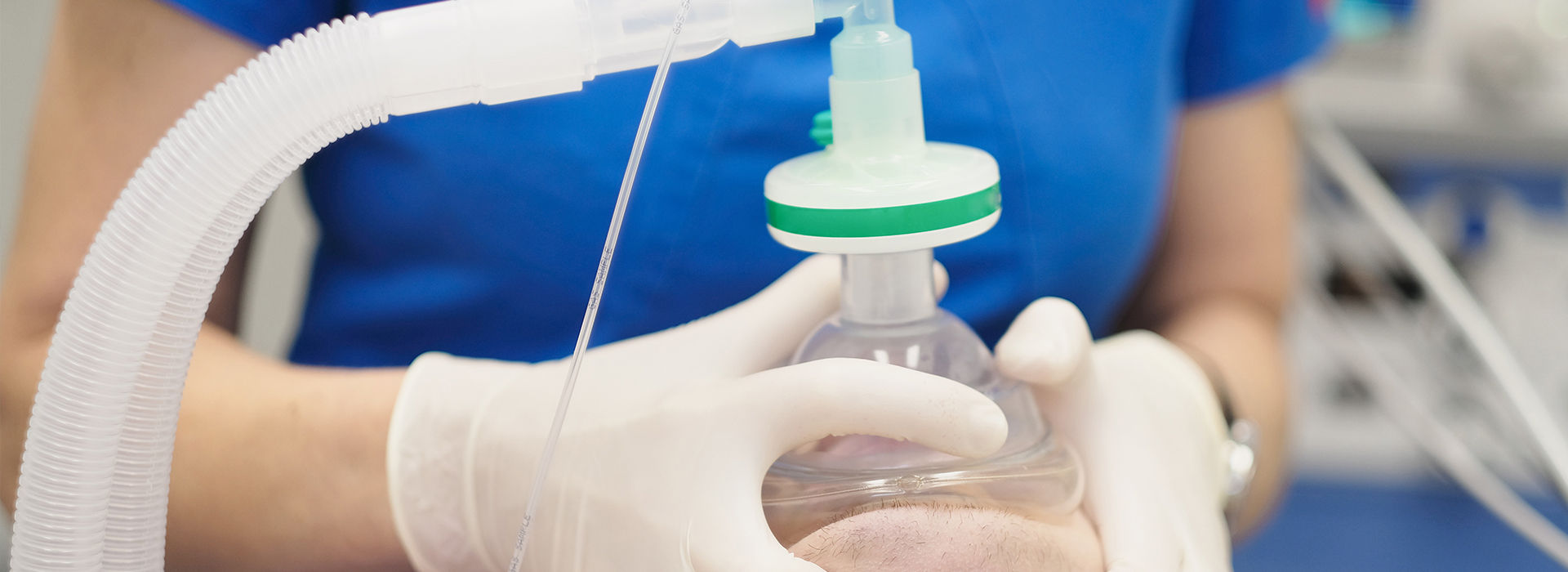
Sedation dentistry is designed to reduce anxiety, block bothersome stimuli, and create a calm environment for dental care. Depending on the technique used, patients may feel lightheaded and peaceful or drift into a deeper state of relaxation. Importantly, sedation is not a replacement for appropriate local anesthesia — it’s a complementary tool that enhances comfort while the dentist manages pain at the treatment site.
One of the key advantages of sedation is its ability to change perception of time and discomfort. Patients frequently report that longer appointments feel shorter and less stressful when sedation is used. This can be particularly helpful for extensive restorative work where multiple procedures can be completed in fewer visits, minimizing the emotional and logistical burden of repeated appointments.
Clinicians tailor sedation to each patient’s needs by evaluating medical history, current medications, and the type of dental work required. The goal is always predictable, safe relaxation that allows procedures to proceed smoothly while keeping vital signs stable and the airway protected. Proper planning and monitoring are the cornerstones of a safe sedation experience.
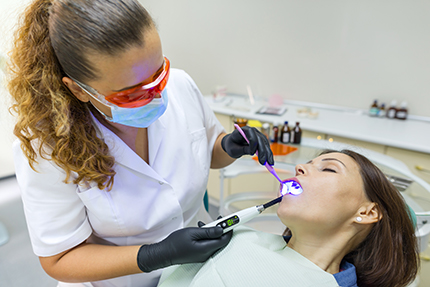
Sedation isn’t just for people with severe phobia — it can serve a range of patients. Those with elevated dental anxiety, a powerful gag reflex, sensitive teeth, or limited ability to sit for extended periods often find sedation makes treatment possible and far more tolerable. Children with special needs and adults with certain cognitive or physical challenges may also be appropriate candidates when the care team determines sedation will improve safety and comfort.
Another common reason to consider sedation is when a patient faces complex or lengthy procedures. Restorative care, multiple extractions, implant surgery, or full-mouth rehabilitation can be difficult to tolerate while fully alert. Sedation helps manage anxiety and movement so the clinician can focus on delivering precise, efficient care with the patient’s wellbeing front and center.
Deciding whether sedation is right requires an honest conversation. Providers review health history, allergies, breathing problems, sleep apnea, and medications that might affect how sedatives are processed. That evaluation ensures the chosen approach balances comfort with safety and aligns with the patient’s overall medical profile.
Sedation exists on a spectrum. On one end are minimal techniques that simply ease nerves, and on the other end are approaches that produce deeper sedation or general anesthesia. For most dental procedures performed in an outpatient dental office, conscious sedation is sufficient and preferred because it allows easy monitoring and quicker recovery while keeping patients comfortable.
Understanding the distinction between conscious sedation and full general anesthesia is important. Conscious sedation keeps patients relaxed and often drowsy, but they remain responsive to verbal cues and breathe independently. General anesthesia, which induces a complete loss of consciousness, is administered and monitored in a hospital setting by an anesthesiologist and is reserved for cases where other methods are inappropriate or unsafe.
At your pre-procedure visit, the dental team will explain the recommended sedation level and why it best fits your needs. That plan will include how the medication is given, how the team will monitor you, and any steps you should take before and after the appointment to ensure a safe outcome.
Conscious sedation is the most commonly used approach in dental offices because it combines safety with effective anxiety control. It can be delivered in several ways: inhaled nitrous oxide, oral medication taken before the visit, or intravenous (IV) sedation administered during the appointment. Each method has predictable effects and specific suitability depending on the patient and the procedure.
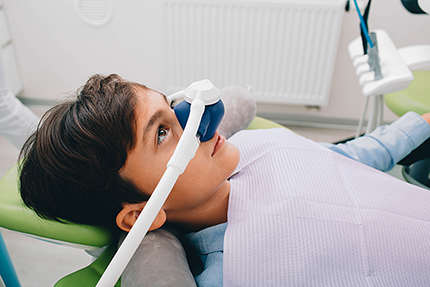
Nitrous oxide, often called “laughing gas,” is inhaled through a small nasal mask and offers rapid onset and quick recovery. It’s ideal for mild to moderate anxiety and for patients who need a calming boost without prolonged aftereffects. A benefit is that the gas is turned off at the end of the appointment and its effects dissipate rapidly, allowing most patients to return to normal activity soon after.
Oral sedatives are taken before the visit and provide a steady, calming effect. IV sedation, by contrast, acts quickly and can be adjusted in real time during treatment, making it valuable for longer or more invasive procedures. Because IV and certain oral sedatives can cause drowsiness and impaired coordination, patients will usually need someone to escort them home and stay with them until they are fully recovered.
Any form of sedation requires vigilant monitoring to keep patients safe. This includes checking blood pressure, heart rate, oxygen levels, and breathing throughout the appointment. The dental team uses modern monitoring equipment and follows established protocols to recognize and respond to changes quickly.
Staff training is also critical: clinicians and support personnel are trained in airway management and emergency procedures, and they maintain certification in basic life support. These safeguards help ensure that sedation creates a calm, controlled environment without compromising patient safety.
Preparing for sedation often involves simple but important instructions, such as fasting for a period before certain sedatives and avoiding specific medications that might interact with sedative agents. The dental team will provide a clear, customized set of pre-appointment guidelines during your consultation.
After the procedure, recovery varies by method. Nitrous oxide wears off quickly, while oral and IV sedation can take longer to clear. Patients should plan quiet activities for the remainder of the day and avoid driving or making important decisions until fully alert. Your clinician will outline any follow-up care and when it’s safe to resume normal activities.
Safety and clear communication are the foundations of responsible sedation care. Before any sedative is administered, clinicians review your health history, medications, and prior experiences with anesthesia or sedation. That discussion helps identify the safest approach and lets the team plan for monitoring and post-procedure instructions.
Continued communication during recovery is just as important. Patients are encouraged to report unusual symptoms, prolonged drowsiness, breathing difficulties, or severe nausea after sedation. The dental office provides guidance on what to expect in the hours and days after treatment and when to seek additional medical attention.
When sedation enables individuals to receive necessary dental care, the long-term benefits extend beyond a single visit: improved oral health, fewer missed appointments, and reduced anxiety over time. Working with a dental team that prioritizes safety, individualized planning, and compassionate communication makes sedation a reliable tool for restoring and maintaining oral health.
If dental anxiety has kept you from getting the care you need, consider discussing sedation options with our team. A Plus Dentistry is committed to helping patients feel comfortable and respected throughout every step of their treatment. Contact us to learn more about sedation dentistry and which approach may be right for you.
Sedation dentistry refers to several techniques used to help patients relax during dental procedures while local anesthesia controls pain at the treatment site. These techniques range from mild calming methods to deeper levels of sedation and are selected based on the procedure, the patient's anxiety level, and medical history. Sedation does not replace local anesthesia; instead, it complements pain control and helps reduce fear and movement so clinicians can work more efficiently.
Sedation can change a patient's perception of time and discomfort, often making longer appointments feel shorter and less stressful. It is commonly used to facilitate routine care, complex restorative work, and procedures that require the patient to remain still for extended periods. The goal is predictable relaxation with careful planning and monitoring to maintain safety throughout the visit.
Sedation dentistry is appropriate for a wide range of patients, not only those with severe dental phobia. People with significant anxiety, a strong gag reflex, sensitive teeth, or difficulty sitting for long appointments frequently find sedation makes care possible and more comfortable. Children with special needs and adults with certain physical or cognitive challenges may also be good candidates when the care team determines sedation will improve safety and cooperation.
Another common reason to consider sedation is when a patient needs complex or lengthy treatment such as multiple extractions, implant surgery, or full-mouth rehabilitation. By reducing anxiety and involuntary movement, sedation helps clinicians complete more procedures safely in fewer visits. A candid conversation about health history and expectations helps determine whether sedation is the right choice for a given patient.
Three common methods of conscious sedation used in dental offices are inhaled nitrous oxide, oral sedatives, and intravenous (IV) sedation. Nitrous oxide, often called laughing gas, has a rapid onset and quick recovery and is well suited to mild to moderate anxiety. Oral sedatives are taken before the appointment and create a steady calming effect, while IV sedation acts quickly and can be adjusted during treatment for longer or more invasive procedures.
Each method has predictable effects and different recovery timelines, so the choice depends on the treatment length, the patient’s medical profile, and personal preferences. The dental team will explain how the medication is given and outline any instructions for before and after the visit. Regardless of the method, monitoring and staff training are essential components of safe sedation care.
Safety is a primary concern with any form of sedation, and modern dental practices follow established protocols and use monitoring equipment to keep patients stable. Typical monitoring includes tracking blood pressure, heart rate, oxygen saturation, and respiration throughout the appointment so clinicians can respond promptly to changes. Staff members involved in sedation maintain training in airway management and basic life support to ensure readiness for emergencies.
Before sedation, clinicians review the patient’s medical history, current medications, allergies, and any previous reactions to anesthesia to choose the safest approach. During recovery, the team continues to observe the patient until they meet objective criteria for discharge or transfer, and clear post-procedure instructions are provided to support safe healing at home.
Disclosing a complete medical history is essential before any sedative is administered, including details about chronic conditions, recent hospitalizations, and sleep-disordered breathing such as sleep apnea. You should also list all prescription and over-the-counter medications, herbal supplements, and any substance use because these can interact with sedatives or affect airway control. Inform the team about past experiences with anesthesia, allergies, and any history of adverse reactions to medications.
Honest communication helps the dental team select the appropriate sedation level and timing and plan necessary monitoring or precautions. If you have concerns about breathing, heart conditions, pregnancy, or other health issues, those topics will be addressed in the planning conversation to ensure safety. The clinician may also coordinate with your medical providers when complex medical issues are present.
Preparing for a sedation appointment typically involves several straightforward steps to reduce risk and promote a smooth experience, such as following fasting instructions when required and avoiding certain medications that might interact with sedatives. The dental team will provide written pre-appointment guidelines tailored to the chosen sedation method, including when to stop eating and drinking and whether to take regular medications the morning of the procedure. Patients should arrange for a responsible adult to drive them home and stay with them if oral or IV sedation is used, because coordination and judgment can be temporarily impaired after the appointment.
On the day of the procedure, wear comfortable clothing and avoid heavy makeup or strong fragrances, which can interfere with monitoring or cause discomfort. Bring a list of current medications and any relevant medical documentation, and arrive a few minutes early to complete consent and safety checks. Clear communication and adherence to pre-procedure instructions contribute directly to a safer, more predictable sedation experience.
Recovery varies by the type and depth of sedation used: nitrous oxide wears off rapidly and most patients return to normal activity quickly, while oral and IV sedatives may produce drowsiness for several hours. Clinicians monitor patients until they meet recovery criteria and provide specific guidance about rest, activity restrictions, and when it is safe to drive or return to work. It is common to feel sleepy or a bit foggy for the remainder of the day after stronger sedatives.
Patients should avoid alcohol, heavy exertion, and making important decisions until they are fully alert, and they should follow any written instructions about medications, wound care, or signs of complications. If prolonged or unusual symptoms occur—such as breathing difficulty, severe nausea, or excessive bleeding—the office should be contacted promptly. Routine follow-up ensures that procedures healed as planned and that any concerns are addressed.
Sedation can be an effective tool to help children and patients with special needs receive necessary dental care, but safety considerations are particularly important in these groups. The decision to use sedation is individualized and depends on the child’s age, medical history, behavioral needs, and the complexity of the dental work. Pediatric dosing and monitoring differ from adult protocols, and clinicians who treat children follow pediatric sedation guidelines to ensure appropriate selection and safety.
For patients with special needs, the care team evaluates cognitive and physical factors that might affect cooperation and airway safety, and they may coordinate with guardians and other healthcare providers to develop a comprehensive plan. Clear communication, careful monitoring, and staff trained in managing pediatric and special-needs patients help create a safer environment for delivering dental treatment under sedation.
Medical conditions such as cardiovascular disease, respiratory disorders, liver or kidney impairment, and sleep apnea can influence which sedation methods are safe and appropriate. Many prescription and over-the-counter medications, as well as herbal supplements, can interact with sedatives to increase or prolong their effects, so an accurate medication list is critical. The dental team uses this information to adjust dosing, choose safer agents, or recommend additional monitoring during the procedure.
When complex medical issues are present, clinicians may consult with a patient’s primary care physician or a specialist to coordinate care and mitigate risks. In some cases, deeper levels of sedation or general anesthesia are delivered in a hospital setting under the supervision of an anesthesiologist to provide a higher level of support and monitoring. The overarching goal is to balance comfort with patient safety through individualized planning.
Determining the right level of sedation begins with a pre-procedure consultation in which the dental team reviews your medical history, anxiety level, and the specifics of the planned treatment. Conscious sedation options typically suffice for most outpatient dental procedures because they allow monitoring while keeping patients responsive and breathing independently. If a procedure is particularly long, complex, or if medical factors require it, a deeper level of sedation or hospital-based anesthesia may be recommended.
During the consultation you should feel empowered to ask questions about the expected effects, monitoring protocols, recovery timeline, and any alternatives to sedation. The team will outline a clear plan explaining why a particular approach is recommended and what steps will be taken to ensure a safe experience. For personalized guidance about sedation and to discuss options in detail, patients can speak with the team at A Plus Dentistry to schedule a consultation.
Quick Links