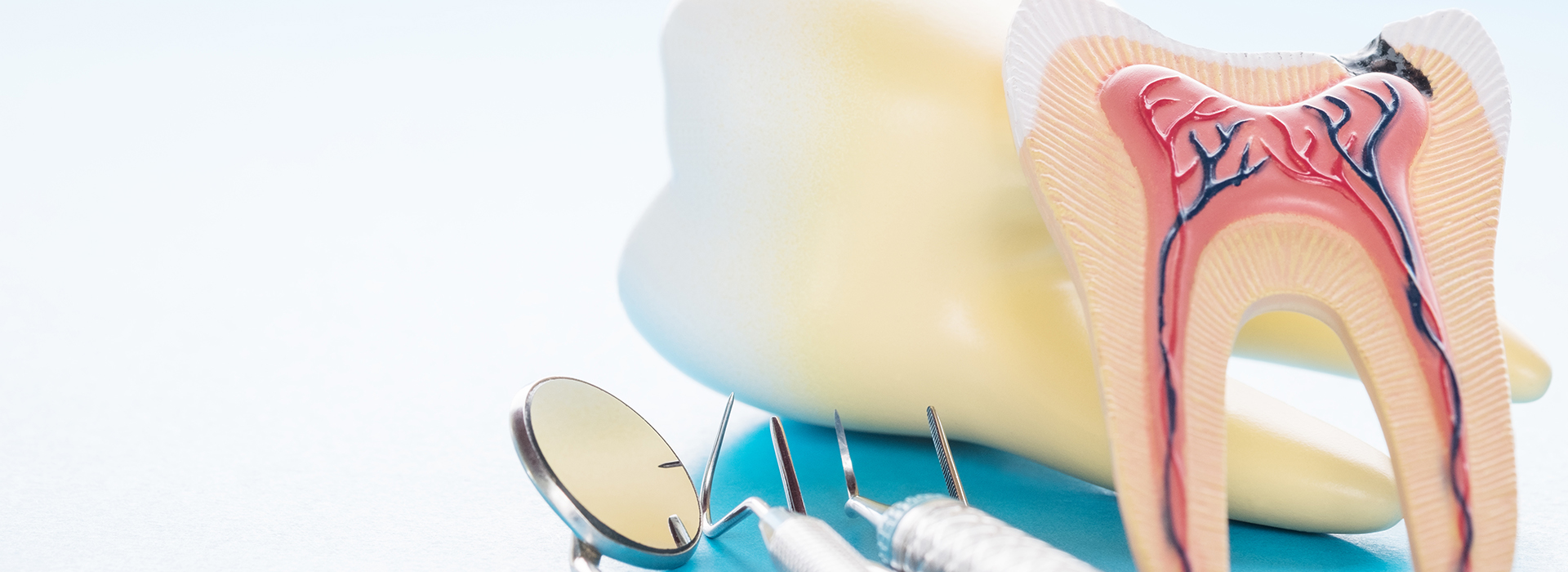
When a dentist recommends a root canal, it’s understandable to feel uneasy — but there’s no cause for alarm. Modern root canal therapy is a predictable, pain-relieving treatment that often feels no different than having a routine dental filling. In many cases, root canal treatment is the best option for stopping toothache, eliminating infection, and keeping your natural tooth in place.
At the office of A Plus Dentistry, we combine up-to-date technology with a gentle approach to help patients protect their smiles. Comfort, clear communication, and clinical excellence guide our care so you can move forward with confidence when a tooth needs attention.
Keeping your natural tooth whenever possible preserves chewing function, maintains facial structure, and protects the surrounding teeth from shifting. Root canal therapy removes diseased tissue inside the tooth while leaving the outer structure intact, so you can continue to eat, speak, and smile naturally.
Thanks to advances in instruments and materials, long-term success rates for root canal treatment are very high. When performed and restored properly, treated teeth can remain useful for many years — often for a lifetime. Choosing conservative treatment that retains tooth structure is usually better for your oral health than extraction when the tooth is otherwise restorable.
Opting for root canal therapy also helps avoid the bone loss and replacement challenges that can follow a missing tooth. By keeping the root structure in the jaw, you preserve the support that keeps adjacent teeth healthy and aligned. In short, saving the tooth when feasible supports both function and long-term oral wellness.

Inside every tooth is a small chamber that contains the dental pulp — soft tissue made up of nerves, blood vessels, and connective tissue. When decay progresses deep into the tooth, trauma occurs, or a previous restoration fails, the pulp can become inflamed or infected. Left untreated, that infection can spread to the tooth root and surrounding bone.
Not all pulp problems begin with dramatic pain. Some develop gradually and are first noticed during a routine exam or on an X-ray. Other times the first clue is sensitivity to hot or cold, a lingering ache, or a dull throb that comes and goes. Paying attention to changes in how a tooth feels helps catch issues earlier, when treatment is most straightforward.
Several common signs can indicate that the inner tissues of a tooth may be compromised. If you notice one or more of the following, it’s wise to seek an evaluation so an appropriate treatment plan can be developed without unnecessary delay.
Although not every instance of dental discomfort indicates the need for root canal therapy, some of the warning signs that you might require this procedure include the following:
Severe or persistent tooth pain — especially pain that wakes you at night — often signals deep decay or an inflamed nerve. This type of discomfort is one of the most common reasons patients ultimately require root canal therapy.
If hot or cold foods and drinks produce sharp or lingering sensations, the pulp may be irritated. While occasional sensitivity is common, prolonged or intense reactions suggest the need for professional evaluation.
Biting pressure that causes pain, or pain when the tooth is lightly tapped, can indicate inflammation or infection in the tooth’s internal structures. These symptoms deserve prompt attention.
Discoloration can occur when the internal tissues have been damaged. A darkened tooth doesn’t always hurt, but it may be a sign that the pulp is no longer healthy and should be evaluated.
Trauma that chips or cracks a tooth can expose or injure the pulp. Even when the damage seems minor, the internal tissues can be affected and lead to pain or infection if not treated.
Swelling near a tooth often points to an infection that may be forming an abscess. In some cases the infection drains on its own, but professional care is still essential to address the source.
Infections that reach the supporting bone can reduce stability and create mobility. Treating the infection and restoring the tooth can often allow healing and return the tooth to normal function.
Timely evaluation and treatment make a meaningful difference. When a compromised tooth is treated before the infection spreads, the procedure is usually simpler and healing is more predictable. Waiting can allow the infection to deepen and the surrounding bone to be affected, which may complicate later treatment.
Some teeth with pulp damage are unexpectedly symptom-free, which is why routine exams and X-rays are valuable. Radiographic signs such as changes around the root tip can reveal problems that haven’t yet caused pain, giving your dentist the opportunity to recommend treatment before symptoms escalate.
Prompt care also reduces the risk that an infection will affect other teeth or contribute to broader health concerns. Root canal therapy eliminates the infected tissue within the tooth and creates the conditions for healing — preserving the tooth and protecting overall oral health.
Contemporary root canal treatment is performed with precision instruments and attention to comfort. Local anesthesia numbs the area, and many patients report that the procedure itself is no more uncomfortable than receiving a filling. For those who prefer it, sedation options are available to help with anxiety.
The number of visits needed depends on the tooth and the situation. Some straightforward cases are completed in a single visit; other teeth with complex anatomy or active infection may be treated over two or more appointments. Your dentist will explain the recommended approach based on the condition of the tooth.
During treatment, the clinician gains access to the pulp chamber, carefully removes the diseased tissue, and cleans and shapes the canal system. The canals are then filled with a biocompatible material to seal them and prevent reinfection. Finally, the tooth is prepared for a durable restoration — often a crown — to restore strength and function.
At A Plus Dentistry, patient comfort and clear follow-up instructions are priorities. After a root canal you can expect some mild soreness as the surrounding tissues recover. This is normal and usually manageable with over-the-counter pain relievers as directed; your dentist will advise you if a prescription is needed.
Following treatment, it’s important to protect the treated tooth until it receives its final restoration. A temporary filling may be placed initially, and chewing on that tooth should be avoided until a permanent crown or restoration is completed. This helps prevent fracture and supports a successful long-term outcome.
With good oral hygiene and routine dental checkups, a tooth that has undergone root canal therapy can remain healthy and functional for many years. If you notice persistent pain, swelling, or any concerning symptoms after treatment, seek prompt attention so issues can be addressed early.
After your root canal procedure, you may experience the following:
You may feel numb for an hour or two after the appointment. Take care to avoid biting your lips, cheeks, or tongue while sensation is returning.
Mild to moderate tenderness for a few days is common and usually improves each day. Follow any pain-management recommendations from your dentist.
If an active infection was treated, you may receive a short course of antibiotics. If prescribed, finish the full course as directed to support complete healing.
A tooth with a temporary restoration can be more prone to damage. Avoid hard, crunchy, or sticky foods and try to chew on the opposite side until the permanent crown or restoration is placed.
Good oral hygiene supports healing and helps prevent future problems. Be gentle around the treated tooth at first, then return to your normal routine as comfort allows.
Restoring the tooth with a crown or suitable permanent restoration restores strength and helps the tooth last. Your dentist will recommend the appropriate timing for that final step.
With attentive care and timely restoration, root canal therapy is a reliable way to relieve pain and preserve natural teeth. If you have questions about symptoms you’re experiencing or whether root canal treatment is the right option, please contact us for more information and guidance.
A root canal is a dental procedure that removes diseased or inflamed pulp from inside a tooth to eliminate infection and preserve the natural structure. The pulp contains nerves and blood vessels that can become infected from deep decay, trauma, or a failed restoration. Removing the damaged tissue stops pain and prevents the spread of infection to the root and surrounding bone.
After the pulp is removed, the canal system is cleaned, shaped, and sealed with a biocompatible material to prevent reinfection. A restoration such as a crown is then placed to restore strength and function. Root canal therapy is often the preferred alternative to extraction when the tooth can be predictably restored.
Local anesthesia is used to numb the tooth and surrounding tissues so the procedure is comfortable for most patients. The clinician creates a small access opening to reach the pulp chamber and uses precise instruments to remove infected tissue and shape the canals. Irrigation solutions disinfect the internal spaces and help remove debris and bacteria.
Once cleaned and dried, the canals are filled with a stable, biocompatible material and sealed to prevent bacteria from re-entering. In many cases a temporary restoration is placed initially and a permanent crown is recommended to restore long-term strength. The dentist will explain whether the treatment can be completed in one visit or requires multiple appointments based on the tooth’s condition.
Modern root canal therapy is performed with local anesthesia and techniques that minimize discomfort during the procedure. Most patients report that the treatment feels similar to having a routine filling rather than intense pain. Sedation options are available for patients who feel anxious or prefer additional comfort.
Some mild soreness or tenderness in the days following the procedure is normal as tissues heal, and it is usually manageable with over-the-counter pain relievers as directed. If antibiotics or prescription medication are recommended because of an active infection, follow the dentist’s instructions closely. Contact the office if pain, swelling, or other concerning symptoms persist beyond the expected recovery period.
At A Plus Dentistry, we recommend arriving with a list of current medications and any health conditions so the dental team can plan safe, effective care. Eat a light meal unless your provider advises otherwise, and arrange transportation if you plan to use sedation. Bring any recent dental X-rays if you have them, though the practice will typically take diagnostic images as needed.
Ask questions in advance about the expected number of visits, the type of restoration recommended afterward, and post-procedure instructions so you know what to expect. If you have allergies or a history of adverse reactions to anesthesia or antibiotics, inform the staff before the appointment. Communicating your concerns allows the team to tailor the experience for your comfort and safety.
Immediately after the appointment you may experience numbness until the anesthetic wears off and mild tenderness as surrounding tissues settle. Over-the-counter pain relievers often control discomfort, and your dentist will advise if a prescription is necessary. Avoid chewing on the treated tooth until a permanent restoration is in place to reduce the risk of fracture.
Maintain gentle oral hygiene around the treated area and return for follow-up visits to monitor healing and complete the final restoration. If a temporary filling was placed, follow instructions for care and report any symptoms such as swelling, fever, or increased pain. Most patients return to normal eating and oral care routines within a few days to a week as healing progresses.
With proper treatment and restoration, a root canal-treated tooth can last many years and often remains functional for a lifetime. Success depends on removing infection, sealing the canals effectively, and protecting the tooth with an appropriate restoration such as a crown. Good oral hygiene and regular dental checkups help detect problems early and support long-term outcomes.
Factors that influence longevity include the extent of the original damage, the quality of the restoration, and the patient’s oral health habits. If reinfection, fracture, or other complications occur, retreatment or extraction may be necessary, but these situations are less common when care is timely. Your dentist will discuss prognosis and monitoring strategies tailored to your tooth.
Extraction may be recommended when a tooth cannot be predictably restored, such as when there is extensive structural damage, severe decay that undermines the tooth, or advanced bone loss around the root. If the tooth has a vertical root fracture or the surrounding bone is compromised, saving the tooth may not be feasible. Your dentist will evaluate these factors and explain why extraction might provide a safer long-term solution.
When extraction is chosen, options for replacing the missing tooth—such as dental implants or bridges—can be discussed to restore function and appearance. Preserving jawbone and adjacent tooth health is a priority in treatment planning, so decisions balance immediate needs with future oral health. Shared decision-making ensures the chosen approach aligns with your overall treatment goals.
Yes, reinfection is possible if bacteria re-enter the sealed canal system or if there are untreated areas within complex root anatomy. Infections can also develop if a temporary restoration fails or a permanent restoration is delayed. Regular monitoring and timely placement of the final restoration reduce the risk of reinfection.
If a treated tooth becomes symptomatic again, options include retreatment, apical surgery, or extraction depending on the cause and condition of the tooth. Diagnostic imaging helps identify the source of reinfection and guide the appropriate approach. Prompt evaluation improves the chance of resolving problems while preserving the tooth if feasible.
Patients with dental anxiety have several options to make root canal treatment more comfortable, including nitrous oxide (laughing gas), oral sedatives, and in some cases, intravenous sedation. Our team at A Plus Dentistry will review medical history and recommend the safest option based on your anxiety level and the complexity of the procedure. Local anesthesia is always used to eliminate pain during the treatment.
Sedation reduces awareness and can help patients tolerate longer appointments in a relaxed state, but it does not replace the need for professional monitoring and post-treatment instructions. If you plan to use oral or IV sedation, arrange for someone to drive you home and follow pre-appointment guidelines provided by the practice. Discuss any previous experiences with sedation so the dental team can tailor care to your needs.
Saving a natural tooth maintains chewing efficiency, preserves jawbone support, and prevents neighboring teeth from drifting into the space left by an extraction. Keeping the root in place helps maintain the structural integrity of the dental arch and supports facial contours. Root canal therapy that allows retention of the tooth therefore supports both function and appearance.
Retaining a tooth also reduces the need for more invasive restorative work that may be required after extraction and helps maintain oral biomechanics. Early evaluation and timely treatment increase the likelihood of successful preservation and reduce the risk of complications that can affect adjacent teeth. Your dentist will consider long-term oral health when recommending conservative treatment like root canal therapy.
Quick Links