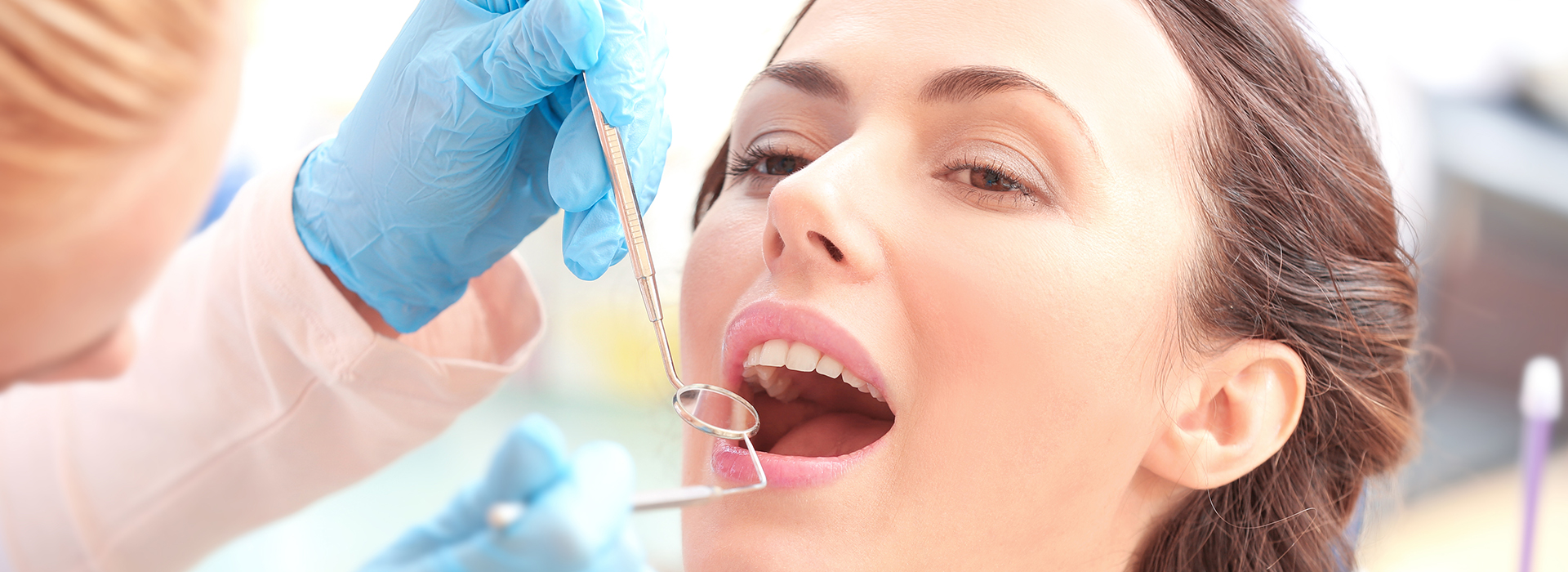
Gum disease is the leading cause of adult tooth loss, yet it often develops quietly and goes unnoticed until significant damage has occurred. Recent public health data show that periodontal problems affect a large portion of adults, making awareness and timely care essential. At A Plus Dentistry, we prioritize clear information and proactive treatment to help patients protect the tissues that hold their smiles in place.
Periodontal disease starts where most oral health problems begin: at the interface between teeth and the surrounding tissues. Bacteria in dental plaque collect along the gumline and, if not removed regularly, harden into calculus (tartar). This bacterial biofilm triggers an inflammatory response in the gums that can progress from mild irritation to a chronic infection affecting deeper structures.
One of the challenges with periodontal disease is that early stages are frequently painless. Because symptoms can be subtle, many people don’t realize there’s an issue until pocketing, recession, or loose teeth appear. That’s why routine dental visits and careful home care are indispensable for catching problems while they’re still reversible.
Recognizing the signs of gum disease allows you to act sooner. If you notice changes in your gums or your bite, seek assessment so a dental professional can determine whether conservative measures will be effective or if more intensive care is required.
Common signs that warrant an evaluation include:
Swollen, tender, or bright-red gum tissue
Bleeding when you brush, floss, or use an interdental cleaner
Gum recession or the sensation that teeth look longer than before
Increased sensitivity to hot, cold, or sweet foods
Persistent bad breath or an unpleasant taste in the mouth
Teeth that feel mobile or shifting positions
Development of new gaps between teeth or a change in how your teeth come together
Partial dentures that no longer fit as they used to
Discharge or pus near the gumline
Discomfort when biting or chewing

Healthy gums do more than anchor your teeth — they contribute to overall well-being. Emerging research has linked periodontal inflammation to several systemic conditions, including cardiovascular issues, diabetes management challenges, and respiratory concerns. While the exact mechanisms continue to be studied, the consistent finding is that uncontrolled oral inflammation doesn’t stay local.
Keeping periodontal disease under control benefits both oral function and general health. Controlling inflammation reduces the bacterial load and the body’s inflammatory burden, which can make it easier to manage chronic health issues and reduce potential systemic risks associated with long-term infections.
Prevention, early detection, and guided treatment form the foundation of periodontal care. Regular dental examinations, professional cleanings, and a personalized home care routine are the most effective tools for maintaining a resilient oral environment that supports overall health.
Gingivitis is the initial, reversible phase of gum disease. It reflects inflammation limited to the gum tissue and has not yet caused irreversible damage to the connective tissues or underlying bone. Common symptoms include redness, swelling, and bleeding during brushing or flossing — signs that the tissues are reacting to a bacterial challenge.
The encouraging news about gingivitis is that it typically responds very well to focused care. Improving plaque removal at home, increasing the frequency of professional cleanings, and sometimes using targeted antimicrobial agents can restore healthy gum tissue within weeks. Early intervention prevents the disease from advancing into stages that require more complex treatment.
Patient education is a crucial part of managing gingivitis. We emphasize techniques that make daily cleaning more effective — including proper brushing mechanics, interdental cleaning methods, and how to establish a sustainable routine. These behavioral adjustments, combined with professional support, are often all that’s needed to reverse early gum inflammation.

If gingivitis is not treated, it can progress to periodontitis, a condition in which the infection extends below the gumline and begins to destroy the connective tissues and bone that hold teeth in place. As the disease advances, periodontal pockets deepen and the structural support around the tooth is compromised, increasing the risk of tooth loss.
Advanced periodontal disease can also alter your bite, create persistent sensitivity, and make routine oral hygiene more difficult. Treatment goals shift from reversal to disease control and structural preservation: stopping active infection, minimizing further tissue loss, and rebuilding support where possible.
Modern periodontal care aims to halt progression and, when feasible, regenerate lost tissues. Techniques such as guided tissue regeneration, bone grafting, and soft tissue grafts can restore form and function in many cases, improving comfort, aesthetics, and long-term stability.
Every case of periodontal disease is unique. A thorough clinical exam, including measurements of pocket depths, assessment of gum recession, and radiographic evaluation of bone levels, forms the basis of a tailored treatment plan. Patient history, medical conditions, and lifestyle factors such as smoking are also considered when choosing the best approach.
Contemporary periodontal therapy blends time-tested procedures with newer technologies. Scaling and root planing remain core treatments for many patients, while adjunctive options — like localized antimicrobials, host-modulating agents, and laser-assisted techniques — can enhance outcomes in selected cases. When tissue loss is significant, regenerative and grafting procedures are used to rebuild the foundation for healthy teeth.
Follow-up care is equally important. Maintenance visits scheduled at appropriate intervals allow clinicians to monitor healing, reinforce home care, and intervene quickly if inflammation recurs. Long-term stability depends on collaboration between the patient and the dental team.
Periodontal treatment paths vary based on disease severity, tissue damage, and individual risk factors. After a comprehensive evaluation, clinicians will outline options, explain the rationale behind each choice, and discuss expected outcomes. The aim is to choose the least invasive, most predictable approach that achieves lasting periodontal health.
When gum disease is recognized early or is limited in scope, conservative measures are often effective. Scaling and root planing (deep cleanings) remove plaque and calculus from below the gumline and smooth the root surfaces to discourage bacterial recolonization. These procedures are performed with comfort measures in place and are commonly paired with enhanced home care and periodic maintenance visits.
Adjunctive treatments such as localized antiseptics or short courses of targeted antibiotics can be used judiciously to reduce bacterial burdens in specific sites. The objective is to eliminate the environmental factors that sustain inflammation so natural healing can occur.
Successful non-surgical therapy reduces pocket depths, improves gum attachment, and makes daily oral hygiene more effective — often preventing the need for surgical intervention.
When periodontal pockets exceed the reach of non-surgical instruments or when significant bone loss is present, surgical procedures may be recommended. Pocket reduction surgery (flap procedures) allows direct access to root surfaces for thorough cleaning and permits reshaping of the underlying bone and soft tissues to create a healthier architecture.
Regenerative techniques — including bone grafting and guided tissue regeneration — are used to encourage the body to rebuild lost structures around teeth. Soft tissue grafts can address recession and improve the aesthetic and functional qualities of the gumline. In appropriate cases, laser-assisted procedures offer a complementary option for reducing pocket depth and managing inflamed tissues.
Postoperative care, maintenance, and close clinical monitoring are essential components of surgical success. With proper healing and ongoing preventive care, many patients maintain improved periodontal stability for years.
At A Plus Dentistry, our approach to periodontal care combines careful diagnosis, evidence-based treatment, and individualized maintenance plans designed to preserve your oral health for the long term. If you have concerns about bleeding gums, persistent bad breath, or loose teeth, please contact us for more information about evaluation and treatment options.
Gum disease begins when bacterial plaque accumulates at the gumline and triggers an inflammatory response in the soft tissues surrounding the teeth. If plaque is not removed regularly, it calcifies into calculus (tartar), which harbors bacteria and makes effective cleaning more difficult. Risk is increased by factors that alter the oral environment or immune response, including poor oral hygiene, smoking, uncontrolled diabetes, certain medications, and genetic predisposition.
Age and systemic health also influence susceptibility, so adults are more likely to develop periodontal problems than children. Periodontal disease can progress quietly for long periods because early stages are often painless, making routine dental examinations critical for people with any risk factors. Identifying and modifying controllable risks helps reduce the chance of progression to more advanced disease.
Early gum disease commonly presents with subtle symptoms such as redness, swelling, and bleeding when brushing or flossing, which are signs of gingival inflammation. Other early indicators include persistent bad breath, an unpleasant taste in the mouth, and increased gum sensitivity to hot or cold foods. Because these signs can be mild, many people assume they are temporary or related to brushing technique rather than an underlying condition.
As disease advances, you may notice gum recession, formation of new spaces between teeth, loose teeth, changes in your bite, or pus near the gumline, which all warrant prompt evaluation. Regular dental visits allow professionals to detect pocketing and bone changes before they become irreversible. Timely attention to early signs makes conservative treatment more likely to succeed.
Diagnosis begins with a thorough clinical examination that includes measuring pocket depths around each tooth, assessing gum recession, and evaluating bleeding on probing to determine the severity of inflammation. Dental radiographs are used to assess bone levels and detect areas of bone loss that are not visible clinically, helping to distinguish between gingivitis and periodontitis. A comprehensive medical and dental history, including habits like smoking and systemic conditions such as diabetes, is collected because these factors influence both diagnosis and treatment planning.
In some cases, clinicians may use adjunctive tests such as microbial sampling or biomarkers to clarify risk or guide targeted therapies, but these are applied selectively based on the clinical picture. After the assessment, clinicians will discuss findings, outline reasonable treatment options, and recommend a maintenance interval tailored to your needs. At A Plus Dentistry, clinicians emphasize evidence-based diagnostics to create personalized, effective care plans.
Gingivitis is inflammation confined to the gum tissue and is considered the reversible early stage of gum disease, characterized by redness, swelling, and bleeding without loss of connective tissue attachment or bone. With consistent plaque control and professional cleanings, gingivitis typically resolves and healthy tissue can be restored. No permanent structural damage has occurred at this stage, making early detection and intervention highly effective.
Periodontitis occurs when the inflammatory process extends below the gumline, destroying connective tissue and alveolar bone that support the teeth, which can lead to pocket formation and tooth mobility. Treatment goals for periodontitis shift from reversal to disease control, stabilization, and, when possible, regeneration of lost tissues through surgical and regenerative therapies. Long-term outcomes depend on both clinical treatment and patient adherence to maintenance protocols.
Non-surgical periodontal therapy typically begins with scaling and root planing, a deep-cleaning procedure that removes plaque and calculus from root surfaces below the gumline and smooths roots to discourage bacterial recolonization. These procedures are often performed with local anesthesia and may be combined with adjunctive therapies such as localized antimicrobials, antiseptics, or short courses of systemic antibiotics when clinically indicated. Host-modulating agents and laser-assisted debridement are additional options that may enhance response in selected cases.
Successful non-surgical care reduces pocket depths, decreases inflammation, and improves attachment levels in many patients, making daily oral hygiene more effective. After initial therapy, a structured maintenance schedule is essential to monitor healing and prevent recurrence. In instances where pockets remain deep or tissue loss is extensive, surgical options may be discussed as the next step.
Surgical intervention is considered when non-surgical therapy cannot adequately access deep pockets or when significant bone and soft tissue loss compromise function or aesthetics. Procedures such as pocket reduction surgery (flap procedures) allow clinicians to gain direct access to root surfaces for thorough debridement and to reshape bone and soft tissues to create a healthier architecture. Soft tissue grafts can address gum recession and improve tissue thickness, while bone grafting and guided tissue regeneration aim to restore lost support around teeth.
Choice of procedure depends on defect type, tooth prognosis, patient health, and treatment goals, and clinicians will explain the expected benefits, risks, and postoperative care. Success of regenerative and surgical therapies relies on meticulous surgical technique, patient healing capacity, and adherence to maintenance visits and home care. Close follow-up after surgery allows early detection of complications and supports long-term stability.
Smoking significantly increases the risk of periodontal disease, accelerates tissue destruction, impairs healing after treatment, and reduces the likelihood of successful outcomes from both non-surgical and surgical therapies. Tobacco use alters the local immune response and blood flow in the gums, masking bleeding signs while promoting deeper infection and bone loss. Quitting smoking is one of the most impactful steps a patient can take to improve periodontal treatment response and long-term oral health.
Diabetes, particularly when uncontrolled, also raises periodontal risk because high blood glucose levels impair immune function and wound healing, making infections more severe and harder to manage. Effective management of systemic conditions in partnership with medical providers improves periodontal prognosis and can reduce complications. Clinicians assess these lifestyle and medical factors when developing individualized treatment plans and maintenance intervals.
During scaling and root planing, your clinician will numb the treatment area with local anesthesia and use manual instruments or ultrasonic devices to remove plaque and calculus from root surfaces below the gumline. The procedure may be done quadrant by quadrant or as needed, and clinicians will take steps to minimize discomfort and ensure thorough cleaning. Treatment time varies with the extent of disease and the number of areas being treated.
After the procedure, it is common to experience mild soreness, sensitivity, and transient bleeding for a few days, which typically improves with recommended home care and analgesics as advised. Your clinician will provide instructions for gentle cleaning, possible antimicrobial rinses, and any medications if indicated, and will schedule follow-up visits to assess healing and measure pocket improvement. Consistent home care and maintenance visits are crucial to consolidate gains achieved by therapy.
Periodontal inflammation contributes to the body’s systemic inflammatory burden, and research has shown associations between periodontal disease and conditions such as cardiovascular disease, poor glycemic control in diabetes, and adverse respiratory events. While causation is complex and studies continue to explore underlying mechanisms, uncontrolled oral infection adds to chronic inflammation and may influence overall health. Addressing periodontal disease reduces local bacterial load and inflammatory mediators that can have downstream effects on general well-being.
For patients with chronic health conditions, controlling periodontal inflammation is an important part of comprehensive care and may improve management of systemic disease. Dental professionals often communicate with medical providers when coordinated care can benefit a patient’s overall treatment plan. Preventive and therapeutic periodontal measures therefore have implications that extend beyond preserving teeth and gums.
Maintenance visits are an essential component of long-term periodontal stability because they allow clinicians to monitor pocket depths, remove new deposits of plaque and calculus, and intervene quickly if inflammation reappears. Frequency of recall is individualized based on disease severity, response to therapy, and risk factors, with many patients requiring professional care every three to six months. These visits also provide opportunities for reinforcement of home care techniques and adjustments to the plan as health changes.
Effective home care—daily brushing with proper technique, interdental cleaning with floss or interdental brushes, and use of recommended adjuncts—reduces bacterial load and supports professional treatment outcomes. Patients who follow a personalized maintenance schedule and communicate openly with their dental team achieve the best chance of preserving natural teeth long term. For guidance and ongoing periodontal management, the team at A Plus Dentistry can help develop a plan tailored to individual needs.
Quick Links