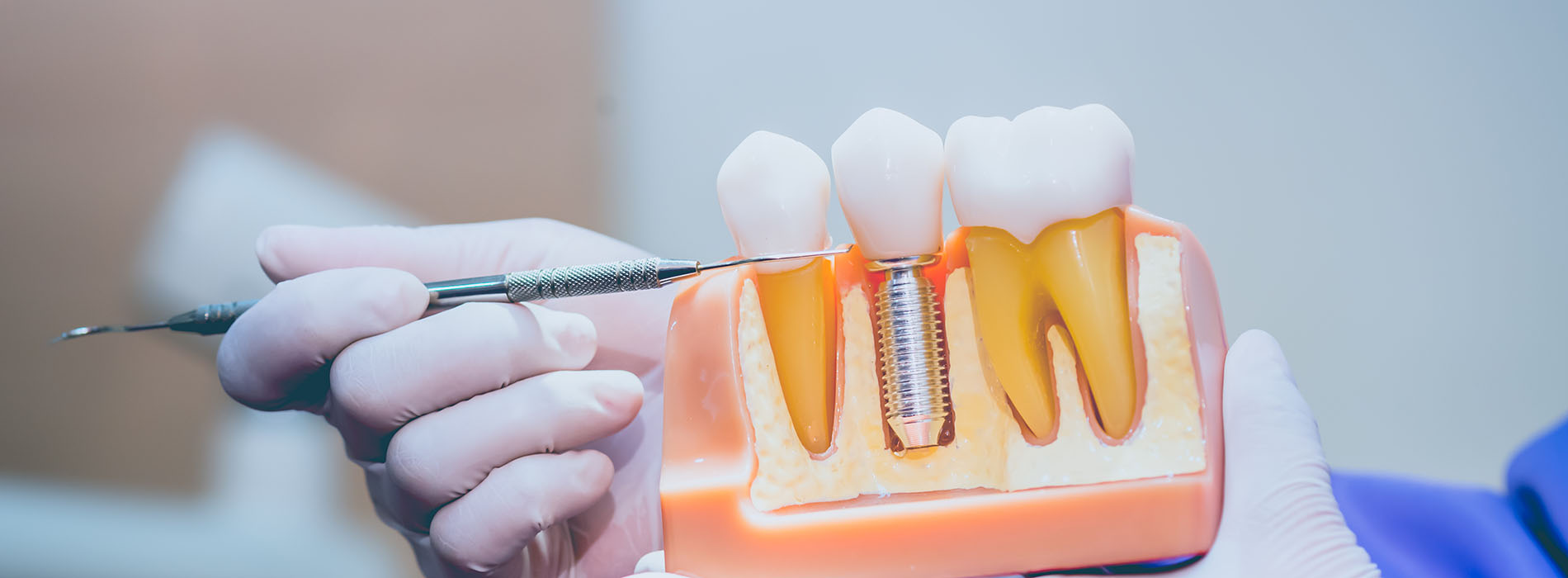
Losing a tooth affects more than just appearance. Missing teeth can change the way you chew, alter speech patterns, and, over time, contribute to changes in facial structure as the jawbone adapts to the absence of a tooth root. Implant restorations are designed to address these functional and aesthetic concerns by rebuilding a stable, tooth-like replacement that interacts with your mouth much like a natural tooth.
Unlike removable dentures that sit on top of the gums, implant restorations rely on a titanium post anchored in the jawbone. This anchored approach helps preserve bone volume and maintain the alignment of neighboring teeth. For patients seeking a durable, long-term solution that restores normal chewing and speaking, implant-supported restorations are often the most predictable option.
At A Plus Dentistry, our goal is to help patients understand how implant restorations can fit into a broader plan for oral health. Whether the objective is to replace a single tooth or to stabilize multiple prosthetic teeth, these restorations offer reliable support for crowns, bridges, and implant-retained dentures while helping protect the integrity of the jaw and surrounding tissues.
The success of an implant restoration depends heavily on osseointegration, the biological process by which the jawbone grows around and bonds to the implant surface. This close integration is what gives the implant the strength and stability needed to hold a crown or bridge under normal chewing forces. Modern implant surfaces and precise surgical techniques have greatly increased predictability and long-term success rates.
Implant planning begins with detailed imaging to evaluate bone quality, anatomical landmarks, and the position of nearby teeth and nerves. Cone beam CT and digital radiography allow clinicians to map the jaw in three dimensions, making it possible to determine the optimal implant length, diameter, and angulation for predictable integration and a natural final result.
After placement, a healing period allows the implant to integrate with the bone. During this time, temporary restorations may be used when appropriate to protect the site and maintain appearance. Once integration is complete, the restorative phase begins: a custom abutment is attached to the implant and serves as the transitional piece between the implant and the visible prosthetic tooth.
An implant restoration isn’t complete until the visible tooth is carefully designed to blend with your smile. Modern restorative dentistry uses lifelike materials—such as high-strength ceramics and zirconia—to create crowns and bridges that match the color, translucency, and contour of adjacent teeth. This attention to detail helps the restoration look and feel like a natural tooth.
Digital workflows, including intraoral scanning and computer-aided design, have transformed how prosthetics are made. Scans capture precise tooth and gum anatomy without the need for traditional impression material, and CAD/CAM milling produces restorations with tight margins and consistent fit. These technologies reduce guesswork and allow for more predictable aesthetics and function.
The restorative team adjusts shape, bite, and shade during the try-in and final seating stages to ensure comfort and proper function. A well-designed crown or bridge not only restores appearance but also distributes biting forces correctly, protecting the implant and neighboring teeth from excessive stress.
The implant restoration journey begins with a thorough consultation and examination. During this visit, clinicians review health history, perform oral exams, and capture diagnostic images. This information helps determine whether an implant is appropriate and identifies any preparatory steps—such as bone grafting or periodontal therapy—that may be necessary to create a stable foundation.
Implant placement is a minor surgical procedure typically performed under local anesthesia, and sedation options are available for additional comfort when needed. After the implant is placed, a healing interval allows the post to integrate with the bone. The timing of the restorative phase varies based on individual healing and the type of implant used, but once integration is confirmed, restoration proceeds with custom abutments and fabricated crowns or bridges.
The final visit focuses on fitting and adjusting the restoration so it functions comfortably within the bite. Our approach emphasizes careful occlusal tuning, soft-tissue adaptation, and patient education so you can return to normal eating and speaking with confidence. Follow-up appointments help ensure that the restoration is functioning well and that gum tissue remains healthy around the implant site.
Caring for an implant restoration mirrors many of the habits that keep natural teeth healthy: daily brushing with a soft-bristled brush, regular flossing or interdental cleaning around the implant, and routine dental checkups. Professional cleanings and periodic examinations allow your dental team to monitor the implant, surrounding bone, and soft tissues for early signs of potential issues.
Peri-implant health depends on both home care and professional maintenance. If plaque accumulates around the restoration, it can lead to inflammation of the soft tissues and, over time, bone loss. Regular assessments help catch changes early so they can be addressed before they compromise the implant.
In some cases, restorations may require maintenance such as tightening of prosthetic screws, replacement of worn crowns, or adjustment of occlusion to accommodate changes in bite. These interventions are part of standard, long-term implant care and help extend the functional life of the restoration while preserving oral health.
Summary and next steps: Implant restorations provide a reliable path to replace missing teeth with solutions that restore function, preserve jawbone, and recreate a natural appearance. With careful planning, modern materials, and ongoing maintenance, implant-supported crowns, bridges, and dentures offer a durable and predictable alternative to removable options. To learn more about how an implant restoration could fit into your treatment plan, please contact us for additional information and to schedule a consultation.
Implant restorations are prosthetic teeth attached to dental implants, a titanium post placed in the jawbone that replaces a missing tooth root. These restorations can support single crowns, multiunit bridges, or implant‑retained dentures and are designed to look, feel, and function like natural teeth. By restoring both form and function, implant restorations help preserve chewing ability and maintain the surrounding dental architecture.
Implant restorations rely on a stable foundation created through careful planning and healing, and they are integrated into a broader treatment plan that considers bone health, gum condition, and overall oral function. At A Plus Dentistry, our team evaluates each case to determine the most appropriate restorative option and to design a final prosthetic that matches your bite and smile. Properly fabricated and seated restorations can provide predictable esthetics and long‑term performance when combined with good maintenance.
Unlike removable dentures that rest on the gums, implant restorations are anchored to the jawbone via implants, which replace the tooth root and provide a fixed foundation. Traditional bridges are supported by adjacent natural teeth and may require modification of those teeth, while implant restorations preserve neighboring tooth structure by standing independently. This root‑level support also helps maintain bone volume and reduces the long‑term bone loss that can accompany tooth loss.
Functionally, implant restorations transmit chewing forces into the bone in a way that more closely resembles a natural tooth, improving bite stability and comfort. Because they are fixed in place, many patients experience improved speech and easier eating compared with some removable options. Treatment selection depends on clinical factors such as bone availability, the condition of adjacent teeth, and the patient’s oral health goals.
The process begins with a comprehensive evaluation that includes oral examination, medical history review, and diagnostic imaging to assess bone quality and anatomical landmarks. Implant placement is a minor surgical procedure performed under local anesthesia, and a healing interval follows to allow the implant to integrate with the bone. During that healing phase, temporary restorations may be used when appropriate to protect the site and maintain appearance.
Once osseointegration is confirmed, the restorative phase begins with attachment of a custom abutment and fabrication of the final crown, bridge, or denture. Digital impressions or conventional impressions capture the exact shape of the tissues and implant position so the laboratory can create a precise prosthesis. The final appointment focuses on fit, esthetics, and occlusal adjustments to ensure the restoration functions comfortably within the bite.
Osseointegration is the biological process by which the jawbone grows around and bonds to the surface of a dental implant, creating a rigid and durable connection. This bone‑to‑implant contact is essential because it provides the mechanical stability that allows the implant to support biting forces without micromovement. Successful osseointegration is a key determinant of long‑term implant success and helps prevent loosening and failure of the restoration.
Factors that influence osseointegration include bone quality and quantity, surgical technique, implant design and surface characteristics, and the patient’s healing capacity. Clinicians verify integration through clinical evaluation and imaging before proceeding with the final restoration, and careful post‑operative care reduces the risk of complications that could interrupt the process.
Modern implant restorations commonly use high‑strength ceramics such as zirconia or layered porcelain fused to a ceramic substructure for crowns, chosen for their esthetic properties and biocompatibility. Abutments are often made of titanium or zirconia; titanium provides strength and proven clinical performance while zirconia offers superior translucency for anterior esthetics. Material selection balances durability, tissue response, and the desire to achieve a natural appearance that matches adjacent teeth.
Custom abutments and CAD/CAM–fabricated restorations allow precise control over emergence profile, margin fit, and occlusal form, which supports soft‑tissue health and prosthetic longevity. Your restorative team will recommend materials based on the location of the implant, esthetic demands, and functional requirements to create a restoration that integrates seamlessly with your smile.
Good candidates are generally adults in good overall health with adequate bone to support an implant and healthy gums free of uncontrolled periodontal disease. Patients should be committed to maintaining excellent oral hygiene and attending regular dental follow‑up visits, since home care and professional maintenance are critical for implant health. Certain medical conditions or habits, such as poorly controlled diabetes or heavy tobacco use, may affect candidacy and require additional evaluation or risk‑reduction measures.
A thorough clinical assessment, including three‑dimensional imaging when appropriate, helps determine whether bone grafting, sinus augmentation, or periodontal therapy is needed before implant placement. The treatment plan is individualized to address any preparatory steps so that implants have the best possible environment for integration. Your restorative team will discuss alternatives and preparatory options during the consultation to reach a safe, predictable plan.
As with any surgical and restorative procedure, implant therapy carries potential risks, including infection, peri‑implantitis (inflammation around the implant), nerve or sinus involvement in certain anatomical situations, and mechanical issues such as screw loosening or prosthetic wear. Early infection or excessive loading during healing can compromise osseointegration, while long‑term soft‑tissue inflammation can contribute to bone loss around the implant. Awareness of these risks allows clinicians to plan interventions that minimize their likelihood.
Complications are managed through prompt diagnosis, targeted treatment, and preventive strategies; for example, peri‑implant soft‑tissue inflammation is treated with professional debridement, improved home care, and, when necessary, localized therapy. Mechanical problems such as loose components or worn crowns can usually be corrected chairside or by the dental laboratory. Regular monitoring and timely intervention are key to preserving implant health and restoring function when issues arise.
Daily care for an implant restoration includes brushing twice a day with a soft‑bristled brush and cleaning between teeth and around the implant with floss, interdental brushes, or other recommended interdental aids. Gentle but thorough removal of plaque along the implant margin is essential to prevent soft‑tissue inflammation and long‑term bone loss. Using nonabrasive toothpaste and avoiding excessive force when cleaning helps protect restorative materials and surrounding tissues.
In addition to home care, maintaining routine dental visits for professional cleanings and implant assessments is vital; dental hygienists use instruments designed to clean around implants without damaging the prosthesis. Your clinician can demonstrate the most effective interdental tools for your specific restoration and provide a tailored maintenance schedule to support long‑term success.
Three‑dimensional imaging such as cone beam computed tomography (CBCT) provides detailed views of bone volume, nerve positions, and sinus anatomy, enabling safer and more precise implant placement. Intraoral scanning and digital impressions capture accurate records of soft‑tissue contours and implant positions, which streamline laboratory communication and reduce the need for remakes. These digital tools allow clinicians to plan implant size, angulation, and prosthetic emergence with greater predictability.
Digital workflows also facilitate guided surgery and CAD/CAM fabrication of custom abutments and restorations, improving fit and esthetics while shortening turnaround times. By combining imaging and digital design, the restorative team can anticipate challenges and deliver prosthetics that align closely with the planned outcome. A Plus Dentistry integrates these technologies into treatment planning to support consistent, predictable results and a smoother patient experience.
Ongoing maintenance includes regular professional evaluations and cleanings at intervals recommended by your clinician to monitor tissue health, bone levels, and the integrity of the restoration. During maintenance visits, the dental team checks occlusion, inspects for signs of wear or loosening, and assesses peri‑implant tissues for inflammation or recession. Radiographic review at periodic intervals helps detect early bone changes that may require intervention.
Patients should report any changes such as persistent soreness, mobility, or draining around the implant so that issues can be addressed promptly. Routine maintenance combined with excellent home care helps protect the implant and surrounding structures, and timely corrective procedures—such as prosthetic tightening, crown replacement, or periodontal therapy—support long‑term function and esthetics.
Quick Links