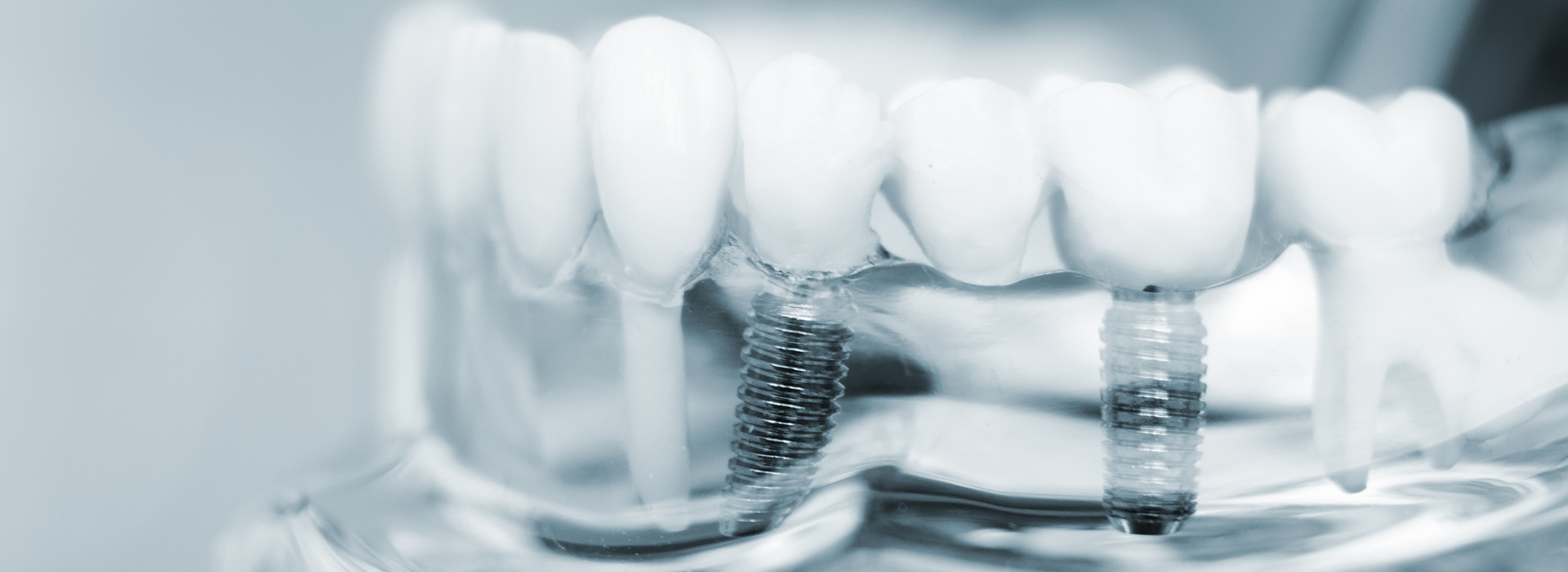
Missing teeth affect far more than just how your smile looks — they change how you chew, speak, and even how your facial tissues support one another. Millions of adults live with gaps from injury, decay, or gum disease, and implant dentistry has evolved into the most predictable way to rebuild missing teeth so they behave like the originals. At A Plus Dentistry, we focus on restoring both form and function so patients can enjoy eating, speaking, and smiling without hesitation.
Implants replace the tooth root with a small, biocompatible post that bonds with the jawbone. That root-like support is what lets implant restorations feel secure and perform naturally, from single crowns to full-arch solutions. Because they integrate with bone, implants also help preserve facial structure and prevent the gradual bone loss that follows tooth loss.
Whether you have lost a single tooth or need a plan for a greater number of missing teeth, modern implant options make it possible to tailor treatment to your goals. In many cases, implants allow replacement without altering healthy neighboring teeth — a conservative approach that protects your long-term oral health.

What sets implants apart is their ability to anchor restorations in the jaw the way natural tooth roots do. This anchorage provides a level of stability that removable options cannot match, so implants eliminate many common frustrations such as shifting, clicking, or the need for adhesives. The result is a restoration that feels anchored and allows you to eat most foods comfortably.
Implant-supported restorations can be designed to match the shape, color, and contour of your natural teeth. Crowns and bridgework attached to implants are crafted to blend with surrounding teeth so that both aesthetics and function are addressed. For full-arch replacements, implant-supported prostheses can be fixed in place or designed to be removable for cleaning — giving a balance between permanence and hygiene access depending on the case.
Compared with older methods, implants often require less compromise of healthy tooth structure. Instead of grinding down adjacent teeth to support a bridge, an implant stands independently, preserving neighboring teeth and providing long-term support for the restoration above it.
A dental implant is typically made from medical-grade titanium or a high-strength ceramic, both chosen for their compatibility with bone and soft tissues. These materials resist corrosion and encourage osseointegration — the biological process where bone grows tightly around the implant surface. That secure union is the foundation of predictable implant performance and longevity.
Implants are composed of three basic parts: the implant body (the part placed in bone), an abutment (the connector), and the prosthesis (crown, bridge, or denture). Each component is selected and shaped to meet both functional demands and aesthetic goals, resulting in a restoration that behaves much like a natural tooth.
Careful selection of materials and components reduces the risk of complications and supports stable outcomes. Advances in implant surface technology and restorative materials have helped increase long-term success rates and enabled clinicians to treat a wider range of cases with confidence.
Predictable implant results start with thorough planning. Modern imaging, such as 3D cone-beam CT scans, allows your clinician to evaluate bone volume, nerve positions, and sinus anatomy before any surgery, making placement more precise and safer. A customized plan considers the number of implants needed, implant size and position, and the type of final restoration that will best meet your needs.
Surgery to place an implant is typically performed on an outpatient basis and often involves only local anesthesia; sedation options are available for patients who prefer additional relaxation. After placement, implants go through a healing phase where they integrate with the bone — a process that can take a few months. In many cases, provisional restorations can be provided so patients leave the office with improved function and appearance while the site heals.
Throughout treatment we focus on clear communication and realistic expectations. Every step — from diagnostic imaging to final restoration — is explained so patients understand the timeline, the care involved, and how to protect their investment with routine maintenance and good oral hygiene.
Most adults who are in generally good health and have adequate bone volume can be considered for implants. A comprehensive evaluation of your medical history, oral health, and lifestyle factors helps determine candidacy. Conditions such as uncontrolled diabetes or habits like heavy smoking may require additional management before moving forward, but many patients can still be successfully treated with proper planning.
When bone has diminished due to long-standing tooth loss or periodontal disease, grafting procedures can rebuild volume to create a stable foundation for implants. Bone grafts and sinus lifts are common adjunctive treatments that make implant placement possible for patients who might otherwise lack sufficient support.
Age alone is not a contraindication; rather, long-term health and oral conditions guide decisions. The goal is to develop a personalized plan that balances predictability with the patient’s goals for comfort, function, and appearance.
Implant placement is a stepwise process: local anesthesia and, if chosen, sedation are provided; the implant is positioned precisely in the jaw; and an abutment or healing cap is placed to shape surrounding tissue. Post-operative instructions include measures to manage swelling and maintain oral hygiene while the site heals. Discomfort is generally manageable with over-the-counter or prescribed medications, and most patients return to normal activities within a few days.
Osseointegration — the fusion of bone to the implant surface — is the critical healing phase. Once integration is complete, impressions are taken for the final restoration, and adjustments are made to ensure a harmonious bite and natural appearance. With routine dental care and proper home hygiene, implant restorations can provide many years of reliable service.
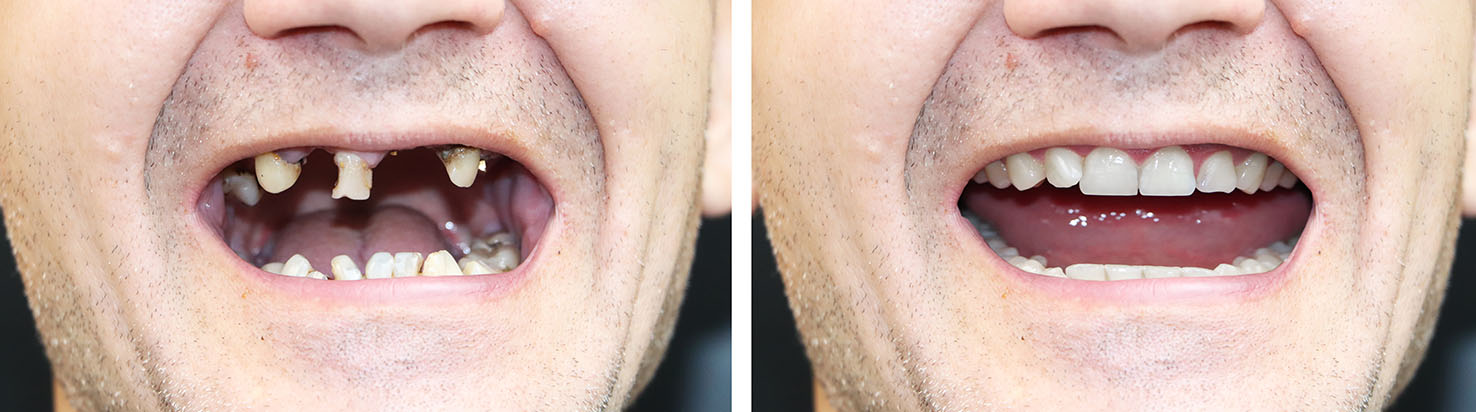
Bone grafting is a straightforward way to rebuild the jaw when volume has been lost. Grafts may use your own bone, donor material, or synthetic substitutes to provide a scaffold for new bone growth. By restoring height and width, grafting improves the long-term stability of implants and helps achieve the ideal placement for both function and esthetics.
Grafting can be performed at the time of extraction, prior to implant placement, or concurrently with implant surgery depending on the clinical situation. Your clinician will explain the rationale, risks, and expected outcomes to help you make an informed decision about adding this step to your treatment plan.
Successful implant dentistry is about more than surgery; it includes careful treatment planning, precise restorative work, and ongoing maintenance. We prioritize clear communication so you understand each phase of care and the habits that contribute to long-term success. Regular checkups and professional cleanings help monitor implants and the health of surrounding tissues over time.
A Plus Dentistry combines modern diagnostic tools, restorative expertise, and a patient-centered approach to help individuals rebuild teeth with predictability and dignity. Our team supports you through every step — from evaluation and imaging to the final restoration and routine follow-up.
If you're considering implants and want to learn how they might restore your smile and oral function, contact us to request more information. We’re happy to explain your options and outline a treatment plan tailored to your needs.
Dental implants are replacement tooth roots made from biocompatible materials such as medical-grade titanium or high-strength ceramic. They are surgically placed into the jawbone where they bond with surrounding bone through a process called osseointegration. This stable integration creates an anchoring foundation that supports restorations and restores chewing and speaking function.
An implant restoration typically includes the implant body, an abutment connector, and a crown, bridge, or denture that sits above the gumline. Each component is selected to meet functional and aesthetic goals so the result blends with your natural teeth. Because implants replace the root as well as the visible tooth, they help maintain facial structure and slow the bone loss that follows tooth removal.
Unlike traditional bridges or removable dentures, dental implants anchor restorations directly to the jawbone, providing superior stability and bite force. Implants restore root function which helps preserve surrounding bone and facial tissues that can deteriorate after tooth loss. Because an implant stands independently, it often avoids the need to alter healthy adjacent teeth to support a prosthesis.
Removable dentures may require adhesives and can shift during eating or speaking, whereas implant-supported options minimize those issues and allow a wider range of foods. Implant-supported bridges and fixed full-arch prostheses can offer long-term durability when combined with proper maintenance. Individual case planning determines whether a removable or fixed solution is best based on oral anatomy and patient preferences.
Many adults are good candidates for implants, but candidacy depends on overall health, oral condition, and sufficient jawbone to support an implant. A comprehensive evaluation of medical history, dental health, and habits such as smoking helps clinicians determine suitability and any steps needed to optimize outcomes. Certain systemic conditions, like uncontrolled diabetes, or heavy tobacco use may require management before implant therapy proceeds.
When bone volume is reduced, common adjunctive procedures such as bone grafting or sinus lifts can often rebuild the foundation needed for implant placement. These procedures expand the number of patients who can receive implants and are planned based on individualized imaging and assessment. Age alone is not a limiting factor; long-term health and oral status guide the treatment approach.
The implant process begins with a detailed consultation that includes 3D imaging, a review of your medical and dental history, and development of a customized treatment plan. Any necessary preliminary care, such as extractions or bone grafting, is coordinated to create the ideal foundation for implant placement. Depending on the case, planning and preparatory steps can span several weeks to a few months before surgical placement.
Surgery to place the implant is typically performed in an outpatient setting under local anesthesia, and sedation is available for patients who prefer additional comfort. After placement, implants require a healing phase during which they integrate with bone; this osseointegration period commonly lasts a few months before the final restoration is attached. At A Plus Dentistry we explain each step and provide provisional solutions when appropriate so patients maintain function and appearance while healing proceeds.
Advanced imaging such as cone-beam computed tomography (CBCT) provides three-dimensional views of bone volume, nerve locations, and sinus anatomy for precise implant planning. Digital impressions and computer-aided planning allow clinicians to select implant size and angulation tailored to each patient's anatomy. When indicated, surgical guides fabricated from the plan can improve placement accuracy and reduce intraoperative surprises.
These technologies support predictable outcomes by minimizing the risk of nerve or sinus injury and by optimizing implant position for both function and esthetics. Comprehensive digital planning also helps determine when adjunctive treatments like grafting are required and how best to stage care. Clear communication of the plan ensures patients understand the rationale and expected timeline.
Bone grafting or sinus lift procedures are considered when the jaw lacks sufficient height or width to securely hold an implant due to long-standing tooth loss, trauma, or periodontal disease. Restoring bone volume creates the structural support needed for predictable implant integration and optimal prosthetic placement. Your clinician assesses bone quality using imaging and will recommend grafting only when it meaningfully improves the prognosis.
Grafting materials can include the patient's own bone, donor bone, or synthetic substitutes chosen for their ability to support new bone formation. Grafts can be placed at the time of extraction, as a staged procedure before implant placement, or simultaneously with implant surgery depending on clinical considerations. Healing timelines vary, but careful planning and follow-up are used to monitor graft maturation before final restoration.
For a single missing tooth, an implant topped with a custom crown replaces the tooth without altering adjacent teeth and restores natural function and aesthetics. Implant crowns are designed to match shape, color, and occlusion to blend seamlessly with surrounding dentition. This conservative approach often provides better long-term support than conventional bridges that rely on neighboring teeth.
When several teeth are missing, implant-supported bridges use strategically placed implants to support multiple crowns without preparing healthy teeth as abutments. For patients missing most or all teeth, full-arch restorations can be delivered as fixed prostheses or as implant-retained dentures that are removable for hygiene. Treatment selection balances permanence, hygiene access, and individual goals for function and appearance.
Home care is essential for implant longevity and includes twice-daily brushing and daily interdental cleaning with floss or brushes to remove plaque around implant restorations. Using nonabrasive toothpaste and paying attention to the gumline around implants helps preserve soft tissue health. Avoiding tobacco and managing systemic health conditions supports healing and reduces the risk of implant complications.
Regular dental exams and professional cleanings allow clinicians to monitor the health of implant-supported restorations and surrounding tissues over time. Routine radiographs and peri-implant evaluations detect early signs of inflammation or bone changes so that interventions can be made promptly. If you grind your teeth, a custom night guard may be recommended to protect the implants and restorations from excessive forces.
Dental implants have a strong safety profile and high long-term success rates when placed and restored with careful planning and technique. As with any surgical procedure, potential risks include infection, temporary or persistent nerve irritation, sinus complications in the upper jaw, and, in rare cases, failure of the implant to integrate. Understanding these risks helps patients make informed decisions and prepares them for appropriate postoperative care.
Thorough preoperative assessment, precise imaging, and adherence to sterile surgical protocols reduce the likelihood of complications. Managing underlying health conditions, avoiding tobacco, and following postoperative instructions further lower risk and support healing. Ongoing maintenance and timely attention to any changes are key to addressing problems early.
Begin with an implant consultation that includes a review of your health, a dental exam, and 3D imaging to evaluate bone and anatomy. Bring any recent dental records and a list of medications to help the team assess your needs and coordinate care. During the visit the clinician discusses treatment choices, sequencing, and what to expect during recovery.
If implants are appropriate, a personalized plan will be created outlining recommended procedures, imaging, and follow-up care tailored to your goals and oral health. A Plus Dentistry in Cumming, Georgia provides the diagnostic tools and restorative expertise to guide patients through each phase of implant therapy. Contact the office to arrange a consultation or to ask questions about the evaluation process and next steps.
Quick Links