
Tooth extraction is not a decision taken lightly. Our goal is always to preserve teeth whenever possible, but there are times when removal is the most responsible option for protecting your oral and overall health. Extractions can prevent spreading infection, stop chronic pain, and create the space needed for proper alignment or future restorations. Understanding why an extraction is recommended helps patients feel more confident about their care plan.
Before recommending removal, we evaluate the whole picture: the tooth’s structure, its supporting tissues, the presence of infection, and how the tooth affects surrounding teeth. We also consider systemic health factors that can impact healing. Every recommendation is tailored to the patient’s individual situation, balancing short-term comfort with long-term function and esthetics.
When extraction is the best path forward, our emphasis is on minimizing discomfort, protecting nearby structures, and planning for the next steps in rehabilitation. Whether the extraction is a simple in‑office procedure or part of a coordinated treatment that involves other specialists, we make sure patients understand the rationale and what to expect at every stage.
Primary teeth that won’t fall out or are damaged
Sometimes a baby tooth remains firmly in place when the permanent tooth is trying to erupt. If a primary tooth becomes ankylosed (fused to the bone) or is badly decayed, it can block the normal development of the permanent tooth and disrupt bite development. Timely extraction can protect future alignment and avoid more complex orthodontic problems.
Permanent teeth that are too damaged to restore
Decay that reaches deep into a tooth or extensive structural loss from previous treatment or trauma can leave a tooth non-restorable. When a tooth cannot be saved with a filling, crown, or root canal, extraction removes a persistent source of infection and pain, reducing the risk to adjacent teeth and tissues.
Teeth with irreparable fractures
A fracture that extends below the gumline or compromises the root often makes restoration impractical. In these cases, extraction protects the health of the jaw and neighboring teeth and paves the way for a predictable replacement option when appropriate.
Advanced periodontal disease
Gum disease that has eroded the bone and connective tissues around a tooth can lead to mobility, pain, and repeated infections. When supporting structures are too compromised to secure a tooth long-term, extraction can stop progressive damage and allow focus on stabilizing the mouth through periodontal therapy.
Wisdom teeth that cause problems
Third molars frequently lack sufficient space to erupt properly, becoming impacted or partially erupted. Impacted wisdom teeth can create pain, infection, and crowding for adjacent teeth. Early removal is often recommended when these teeth threaten oral health or create recurring issues.
Teeth removed as part of orthodontic planning
When there isn't enough space to align teeth properly, selective extraction can be a planned step in an orthodontic strategy to create room and achieve a balanced bite. In such cases, extractions are performed with long-term alignment and function in mind.
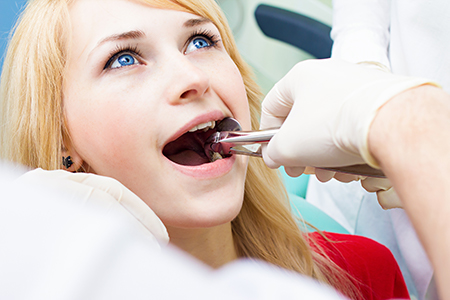
Preparation begins with a careful review of your medical and dental history and a focused clinical exam. We take digital radiographs when indicated to evaluate root shape, adjacent anatomy, and the relationship of the tooth to nearby structures. That information guides whether a tooth can be removed simply or requires a more involved surgical approach.
Local anesthesia is typically used to numb the area; for patients who experience anxiety or need additional comfort, a discussion about sedation options is part of the pre-treatment planning. We will explain any special instructions, such as alterations to medication or the need for preoperative medical clearance, so patients arrive prepared and confident.
Communication is key throughout the procedure. We explain each step in plain language, monitor comfort, and respond to concerns immediately. The extraction itself is performed with precision and care to preserve bone and soft tissue when possible, which helps reduce recovery time and preserve sites for future restorations if needed.
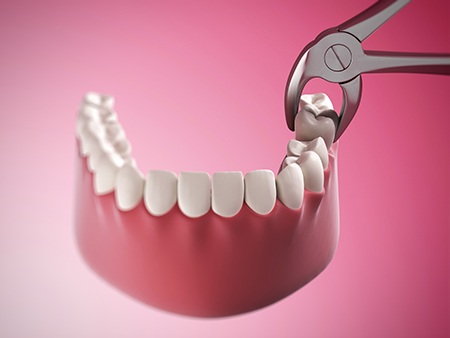
Simple extractions are appropriate when a tooth is fully erupted and the roots are predictable. After effective local anesthesia, the dentist will gently loosen the periodontal ligaments and use forceps to remove the tooth. The goal is to remove the tooth with minimal trauma to surrounding bone and soft tissue so healing can proceed quickly.
Even though the technique is routine, we never rush. We take steps to maximize comfort during and after the appointment, including offering guidance on pain control, wound care, and signs of normal healing versus complications. When sutures are required or a replacement plan is being arranged, we will outline follow-up steps clearly.
Surgical extractions are necessary when a tooth is fractured at the gumline, ankylosed to the bone, impacted beneath the surface, or has an unusual root shape. In these cases, an incision and localized removal of a small amount of bone may be required to access and remove the tooth safely. This approach can also be coordinated with an oral surgeon if complexity warrants referral.
Because surgical cases can involve more tissue manipulation, they often require additional post-operative instructions and possibly sutures. We review healing expectations and any pre- or post-operative medications that may be necessary to reduce the risk of infection and support a smooth recovery.
Healing after an extraction is a predictable process when patients follow clear, evidence-based guidance. The first 24 to 48 hours are focused on controlling bleeding, managing discomfort, and protecting the blood clot that forms in the socket. Simple, consistent measures help reduce swelling and lower the chance of complications like dry socket.
We provide individualized post-operative instructions based on the type of extraction and the patient's health profile. These directions cover activity limits, diet recommendations, wound care, and when to resume routine oral hygiene. If you are taking medications for other health conditions, we coordinate with your medical team as needed to ensure safe recovery.
If concerns arise — such as persistent bleeding, increasing pain after the first few days, or signs of infection — it's important to contact the office promptly so we can evaluate the healing process and intervene when necessary.
Support the clot with light pressure
After your appointment, bite gently on gauze as instructed to help a stable clot form. Change gauze as directed, and avoid vigorous rinsing or spitting on the first day to protect the clot.
Protect numb areas
Until feeling returns, be careful not to chew your lips, cheeks, or tongue. The numbness from local anesthesia can temporarily decrease awareness and lead to accidental bites.
Follow medication instructions
If antibiotics or pain medications are prescribed, take them exactly as directed. Over-the-counter options for mild discomfort can be helpful and should be used according to package guidance or our recommendations.
Protect the healing site
Avoid actions that can dislodge the clot, including drinking through straws, smoking, or spitting forcefully for the first several days. Stick to soft, cool or lukewarm foods and keep well hydrated.
Reduce swelling
Apply an ice pack intermittently during the first 24 hours to minimize swelling. After the initial period, warm compresses may help relieve any remaining stiffness or discomfort.
No tobacco
Smoking interferes with blood clot formation and slows healing. Avoid tobacco products for at least a week to support optimal recovery.
Diet and hygiene
Choose soft, non-irritating foods and maintain oral hygiene with gentle brushing away from the extraction site. When appropriate, a mild saline rinse can help keep the area clean after the first 24 hours.
Attend follow-up visits
If stitches were placed or additional monitoring is needed, keeping scheduled follow-up appointments allows us to confirm proper healing and address any concerns early.
If you notice unusual symptoms such as increased swelling, a persistent bad taste, or prolonged bleeding, contact the office so we can evaluate and, if needed, provide further care.
Removing a tooth can create questions about how the space will be managed going forward. Replacement options range from removable prosthetics to fixed bridges and dental implants. Each choice has its indications based on health, anatomy, and the patient’s long-term goals for function and appearance.
Dental implants are frequently recommended when preserving adjacent teeth and supporting bone is a priority. Fixed bridges can provide a durable option when implants aren’t appropriate, and removable dentures remain a reliable solution for many patients. We discuss timing for replacement as part of the treatment plan so you can make an informed decision at the right stage of healing.
Coordinating extraction with timely replacement can help preserve bone and soft tissue contours and support a predictable restoration. When a staged approach is needed, we outline a clear timeline and collaborate with specialists when complex reconstruction is required.
Your care should be delivered by clinicians who combine technical skill with thoughtful planning and clear communication. At A Plus Dentistry, we focus on conservative decision-making, precise execution, and comprehensive follow-through so that extraction is only one step in a coordinated path toward lasting oral health.
From initial evaluation through healing and restoration, our team works with patients to explain options, manage expectations, and minimize discomfort. We also partner with trusted specialists when a case benefits from additional expertise, ensuring each patient receives the right level of care for their needs.
If you’re facing a tooth that may need removal or you’re planning for replacement after an extraction, we’re here to help. Contact us to discuss your situation, learn about the steps involved, and get clear guidance on the path forward.
Tooth extraction is recommended when preservation jeopardizes oral health, such as uncontrolled infection, severe structural damage, or advanced periodontal support loss. At A Plus Dentistry we prioritize conservative treatments but recommend removal when it prevents spread of disease or preserves overall function. Understanding the rationale helps patients make informed decisions with their care team.
Clinicians evaluate both short-term comfort and long-term outcomes before recommending extraction, balancing the health of adjacent teeth and supporting bone. When extraction is advised, the treatment is planned to minimize trauma and preserve tissue for future restoration when appropriate. Clear communication about risks, benefits, and alternatives is part of each individualized care plan.
We decide whether to save or remove a tooth by combining a clinical exam, diagnostic imaging, and a review of your medical history. Radiographs reveal root morphology, bone levels, and the extent of decay or fracture, while a clinical exam assesses mobility, periodontal health, and symptoms like pain or recurrent infection. Health conditions and medications that affect healing are also considered to reduce the risk of complications.
A tooth is often considered salvageable if it has sufficient crown structure for restoration, healthy supporting bone, and no untreatable infection. When restorative options such as crowns, root canals, or periodontal therapy are unlikely to provide predictable results, extraction becomes the safer, more reliable solution. The decision is made collaboratively, with the clinician explaining alternatives and next steps.
A simple extraction is performed on a fully erupted tooth with predictable root anatomy and usually requires only local anesthesia and forceps to remove the tooth. The procedure is typically quick and involves gentle luxation of the tooth and extraction with minimal bone removal, leading to faster initial healing. Postoperative instructions focus on protecting the blood clot, controlling discomfort, and maintaining oral hygiene around the extraction site.
Surgical extractions are required for teeth that are impacted, fractured at the gumline, ankylosed, or have complex root shapes that cannot be accessed easily. These procedures often involve an incision, elevation of a flap, and selective removal of a small amount of bone to access the tooth, and they may require sutures and a longer recovery period. Complex cases may be coordinated with or referred to an oral surgeon to ensure safe, predictable outcomes.
Before your extraction appointment we review your medical history, current medications, and any conditions that could affect healing, such as diabetes or anticoagulant use. If imaging or medical clearance is necessary, we arrange those steps in advance and provide specific preoperative instructions to help you arrive well prepared. Patients should arrange for transportation if they plan to use sedation and should follow any medication guidance provided by the care team.
On the day of the procedure, avoid smoking and follow instructions about eating if you will have sedation; otherwise, a light meal is typically acceptable before local anesthesia. Bring a list of medications and emergency contact information, and ask any questions you have about the process or aftercare so expectations are clear. Preparing in this way reduces anxiety and helps the appointment proceed smoothly.
Local anesthesia is the foundation for pain control during most extractions, providing targeted numbness so the procedure is comfortable for the patient. For anxious patients or more invasive procedures, additional sedation options such as oral sedatives, nitrous oxide, or intravenous sedation may be offered to increase comfort and reduce awareness of the procedure. The choice of sedation depends on the patient's medical history, anxiety level, and the complexity of the extraction.
Before recommending sedation, clinicians discuss risks, benefits, and fasting or escort requirements to ensure safety and compliance with best practices. Patients receiving moderate or deep sedation will need someone to drive them home and follow post-sedation instructions closely. Care plans are individualized to balance patient comfort with procedural safety.
During extraction the clinician confirms anesthesia, verifies comfort, and proceeds with a step-by-step approach to remove the tooth while protecting surrounding bone and soft tissue. Simple extractions involve controlled loosening and forceps removal, while surgical cases may require incisions and bone removal performed with precision instruments. Throughout the procedure, the team monitors the patient's comfort and addresses questions or concerns as they arise.
After the tooth is removed the socket is inspected, cleaned, and, when necessary, sutured to support healing and preserve tissue contours. The clinician provides clear aftercare instructions and schedules follow-up when indicated to monitor healing or begin restorative planning. Attention to meticulous technique during the procedure helps reduce the likelihood of complications and supports a predictable recovery.
Initial healing focuses on protecting the blood clot, controlling bleeding and swelling, and managing discomfort with appropriate medications and conservative measures. Patients are advised to bite gently on gauze as directed, avoid vigorous rinsing or spitting for the first 24 hours, and use ice intermittently during the first day to limit swelling. Maintaining a soft diet and avoiding actions that could dislodge the clot, such as smoking or using a straw, supports uncomplicated healing.
After the first 24 to 48 hours, gentle saline rinses can help keep the site clean and promote comfort as tenderness subsides. Gradually reintroduce normal oral hygiene while avoiding direct brushing of the extraction site until it is sufficiently healed, and attend any scheduled follow-up visits so the clinician can confirm progress. If pain increases or other concerning symptoms develop, contact the office promptly for evaluation.
While most extractions heal without issue, certain signs may indicate a complication that requires prompt attention, such as severe pain that begins a few days after the procedure, prolonged bleeding, or persistent swelling that worsens over time. A foul taste or discharge, fever, or numbness that does not resolve may also signal infection or nerve involvement that needs evaluation. Early recognition and timely follow-up allow clinicians to treat problems such as dry socket or infection effectively.
If you experience any worrying symptoms, contact the office so the team can assess the situation and recommend appropriate care, which may include in-office treatment, medication, or referral to a specialist. Documentation of your symptoms, including timing and severity, helps the clinician determine the appropriate next steps quickly. Prompt communication helps protect oral health and supports a smoother recovery process.
Replacing a tooth after extraction preserves chewing function, prevents shifting of adjacent teeth, and helps maintain bone volume and facial support. Replacement options include dental implants, fixed bridges, and removable prosthetics, and the optimal choice depends on your oral health, bone anatomy, and long-term goals. Timing for replacement is individualized; immediate, delayed, and staged approaches each have advantages depending on healing and reconstructive needs.
Dental implants are often recommended when preserving adjacent teeth and bone is a priority, and fixed bridges can be appropriate when implant treatment is not indicated. At A Plus Dentistry the team outlines a clear timeline for restoration and coordinates care so that replacement integrates with healing and any additional treatment. Discussing these options before and after extraction helps patients plan for a predictable functional and esthetic outcome.
Wisdom teeth are evaluated using clinical exam and radiographs to determine eruption patterns, impaction depth, and proximity to nerves and sinuses. When third molars cause pain, recurrent infection, damage to adjacent teeth, or threaten orthodontic outcomes, removal is often recommended to protect overall oral health. Early evaluation during the teenage years or early adulthood helps identify problematic wisdom teeth before they cause more complex issues.
Surgical removal of impacted wisdom teeth may require coordination with an oral surgeon when roots are close to nerves or when impactions are complex. The decision to remove is based on current symptoms and the likelihood of future problems, and patients are counseled on what to expect during recovery and any specific aftercare measures. Regular monitoring of asymptomatic wisdom teeth can also be an appropriate alternative when immediate removal is not indicated.
Quick Links