Modern dentistry gives us more options than ever for rebuilding a complete, confident smile. Advances in materials, digital design, and prosthetic techniques mean removable dentures can now be more comfortable, more natural-looking, and longer-lasting than in the past. While fixed restorations such as dental implants and bridgework remain excellent choices for many patients, removable dentures continue to be a dependable solution for restoring function, facial support, and the appearance of a full dentition.
Our approach emphasizes careful planning and individualized care. We consider each patient’s oral health, jaw anatomy, lifestyle, and long-term goals before recommending a denture solution. This allows us to balance practical function with a natural appearance so patients can eat, speak, and smile with confidence.
If you’re exploring options for replacing missing teeth, you’ll find that a well-made denture is more than a set of teeth — it’s a thoughtfully designed appliance that supports oral health and daily life. Below, we explain how tooth loss affects the mouth, what modern dentures are, how they differ, and what to expect when you choose to move forward with treatment.
Losing one or more teeth can feel like an isolated problem, but its consequences often extend beyond the immediate gap. Tooth loss can change how you chew and pronounce certain sounds, which may limit the foods you can comfortably enjoy and affect social interactions. Over time, these functional changes can influence nutrition, digestion, and self-confidence.
Physiologically, the absence of teeth can lead to bone remodeling in the jaws. Without the stimulation that tooth roots provide, the supporting bone can shrink, and the surrounding soft tissues may lose volume. These changes can alter facial contours, making the lower face appear shorter or sunken if not addressed.
Adjacent teeth may also shift toward open spaces, disrupting your bite and creating areas that are harder to keep clean. That drifting can increase the risk of decay and periodontal problems in otherwise healthy teeth. Addressing tooth loss in a timely way helps preserve the remaining dentition and the overall balance of the mouth.
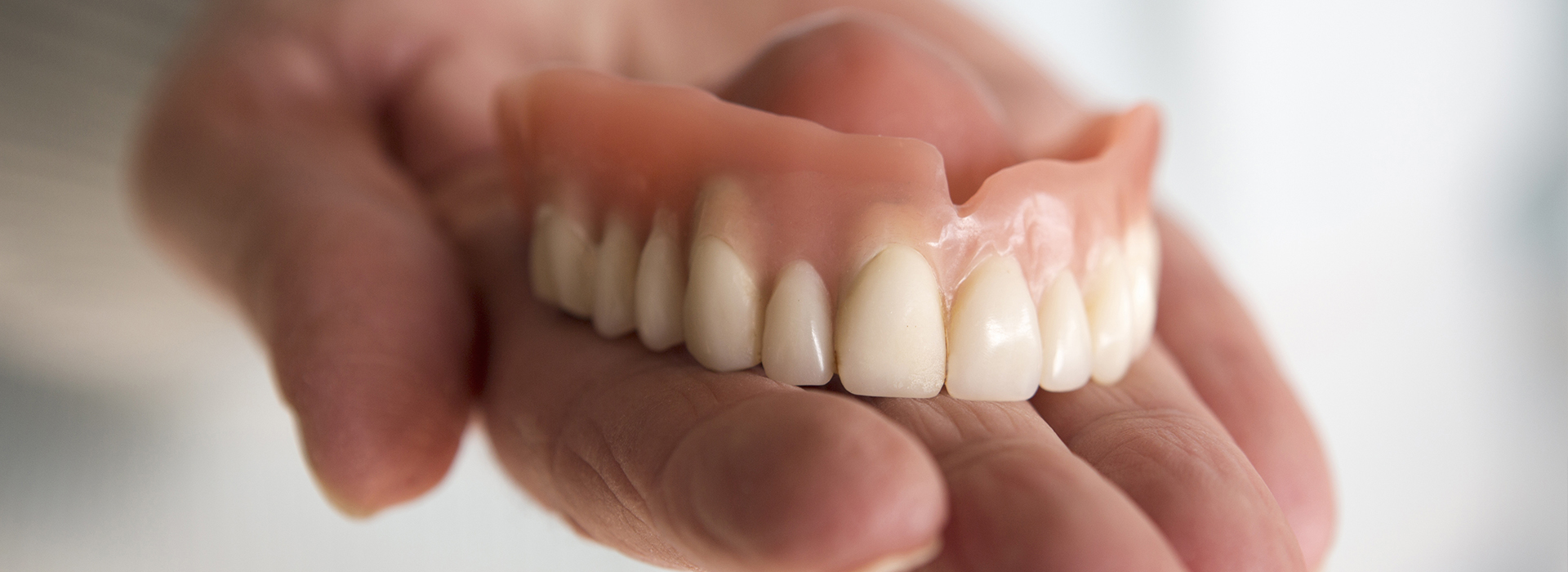
Dentures are removable prosthetic appliances that replace missing teeth and the nearby gum tissue. They consist of lifelike artificial teeth set into a supportive base, carefully contoured to sit comfortably on the gums. The primary goals are to restore chewing function, support facial appearance, and provide a natural smile that fits the patient’s facial proportions.
Because they are removable, dentures make it easy to clean both the appliance and the tissues beneath it. This accessibility helps maintain oral hygiene and monitor the health of any remaining teeth. Removable options are especially versatile when multiple teeth are missing across an arch or when a nonfixed solution better matches a patient’s needs or preferences.
While fixed restorations can feel more like natural teeth, removable dentures offer specific advantages: they can replace many teeth at once, are readily adjustable, and are compatible with a variety of treatment plans. Newer materials and techniques also allow for improved esthetics, stronger bases, and better-fitting prostheses than ever before.
Choosing the right type of denture depends on how many natural teeth remain, the condition of those teeth, the shape of the jaws, and the patient’s functional expectations. In simple terms, dentures fall into two broad removable categories: full (complete) dentures and partial dentures. Within those categories there are variations that address timing, extra support, and specific anatomic needs.
Complete dentures replace all the teeth in an upper or lower jaw. They are shaped to restore occlusion (how the jaws come together) and to support facial soft tissues. When the supporting tissues have healed following extractions, a conventional full denture can be fabricated for a precise, stable fit. That careful timing often yields the best long-term comfort and function.
Immediate dentures
Immediate dentures are placed on the same day as extractions so the patient doesn’t go without teeth during healing. They provide immediate esthetic and functional restoration, though they may require relines or adjustments as the gums and bone remodel in the weeks and months after extractions.
Overdentures
An overdenture gains extra stability by resting on preserved tooth roots or on attachments connected to implants. This approach can help maintain bone volume and improve retention compared with a conventional denture that relies only on tissue contact and suction.
Implant-supported dentures
Implant-supported dentures attach to strategically placed dental implants in the jaw. These provide fixed points of retention and greatly improve chewing efficiency and stability, especially for lower-arch dentures that are otherwise prone to movement.
Partial dentures are designed for mouths where some healthy natural teeth remain. They fill gaps, preserve spacing, and help distribute biting forces more evenly. Partials typically anchor to neighboring teeth using clasps or precision attachments, and modern materials offer options ranging from lightweight flexible resins to robust metal frameworks with acrylic teeth.
A well-designed partial not only restores appearance and chewing ability but also prevents unwanted tooth drifting and helps maintain the overall alignment of the dental arch. The choice of framework and attachment style will reflect the location of missing teeth, the condition of adjacent teeth, and patient preferences for comfort and maintenance.

Creating a denture that looks good and performs well begins with a detailed evaluation. We review your medical and dental history, examine the condition of any remaining teeth and supporting tissues, and often use imaging to assess bone levels and jaw relationships. This diagnostic step guides whether extractions, pre-prosthetic procedures, or implant placements are advisable.
The fabrication process typically involves precise impressions, multiple try-in appointments, and careful color and form selection for the teeth. These steps let us fine-tune how the prosthesis fits, how it supports facial contours, and how the bite feels during speech and chewing. Attention to these details helps reduce sore spots and minimize the need for extensive adjustments later on.
Communication between the dental team, the laboratory technician, and the patient is essential. Treatment planning is collaborative: we discuss expectations, describe likely timelines for healing and adjustments, and outline comfort and care strategies so patients know what to expect at each stage.

Wearing a new denture is an adjustment. In the first days or weeks you may notice increased saliva, mild soreness, or small changes in speech. These reactions are normal. With practice—speaking aloud, starting with soft foods, and gradually increasing chewing — most people adapt quickly and regain comfortable function.
Proper daily care preserves the appearance and hygiene of the appliance. Rinse dentures after meals, brush them with a soft denture brush, and soak them overnight in water or a recommended cleansing solution. It’s equally important to care for any remaining natural teeth and the health of the gums with regular brushing and dental checkups.
Over time, the shape of the gums and underlying bone can change. Periodic professional evaluations ensure the denture continues to fit properly; adjustments, relines, or repair work can restore comfort and function. In cases where additional retention is needed, attachments or implant support may be discussed as long-term alternatives.
When you are ready to consider dentures, our team combines modern techniques with careful, patient-centered planning to achieve predictable, natural results. A Plus Dentistry brings experience and attention to detail to every step of the process, from initial evaluation through ongoing maintenance.
If you’d like to learn more about denture options and which approach is best for your situation, please contact us for more information. We’re happy to answer questions and help you explore the solutions that will restore comfort, function, and confidence to your smile.
Dentures are removable prosthetic appliances that replace missing teeth and the adjacent gum tissue to restore chewing, speech, and facial support. They consist of lifelike artificial teeth set into a supportive base that is contoured to fit the gums and oral anatomy. Modern dentures use improved materials and design methods to enhance esthetics, fit, and durability compared with older prostheses.
By restoring occlusion and biting surfaces, dentures help patients eat a wider variety of foods and speak with clearer articulation. They also support facial soft tissues, which can reduce the appearance of a collapsed or sunken lower face after tooth loss. Regular professional care and periodic adjustments help maintain function and comfort over time.
There are two broad removable categories: complete (full-arch) dentures and removable partial dentures, each tailored to the number of missing teeth and the condition of remaining teeth. Complete dentures replace all teeth in an upper or lower jaw and are designed to restore bite relationships and facial contours, while partial dentures fill gaps where some healthy teeth remain and typically use clasps or precision attachments for retention. Within these categories are variations such as immediate dentures placed at the time of extractions, overdentures that rest on preserved roots or implant attachments, and implant-supported dentures that anchor to surgical implants for added stability.
Material and framework choices also differ: partials may use flexible resin or metal frameworks depending on strength and esthetic needs, while full dentures commonly feature acrylic bases and a range of tooth materials chosen for durability and appearance. The selection depends on oral anatomy, functional expectations, and long-term treatment goals. A careful diagnostic evaluation helps determine which option best balances comfort, retention, and maintenance for each patient.
Good candidates for dentures include people who are missing multiple teeth, have significant tooth decay or periodontal disease that precludes saving certain teeth, or prefer a removable solution for replacing an entire arch. The decision also depends on jawbone condition, the health of any remaining teeth, overall medical history, and the patient’s lifestyle preferences for maintenance and oral hygiene. Patients with certain systemic conditions or limited manual dexterity can still be candidates, but the treatment plan may be adapted to address those considerations.
A thorough clinical exam and imaging allow the dental team to evaluate bone levels, soft tissue health, and bite relationships before recommending dentures or alternative options such as implant-assisted prostheses. When teeth are present that can help support an overdenture, preserving those roots can be beneficial for retention and bone preservation. Open communication about functional goals and expectations ensures the chosen solution aligns with the patient’s needs.
Implant-supported dentures attach to dental implants placed in the jaw, providing fixed points of retention that greatly improve stability and chewing efficiency compared with conventional removable dentures. This is especially valuable for lower-arch prostheses, which are more prone to movement when they rely only on tissue contact and suction. Implant attachments can range from locators and bars to fixed hybrid designs that function more like permanent restorations.
Because implants stimulate the underlying bone, they can slow bone resorption and help preserve facial contours over time, which contributes to long-term fit and comfort. The surgical and restorative phases require careful planning and adequate healing time, and not every patient is an immediate candidate for implants without preparatory procedures. A diagnostic workup determines whether implant-assisted options are feasible and which design will best meet functional and esthetic goals.
Planning a custom denture begins with a comprehensive evaluation that includes medical and dental history, an oral exam, and imaging to assess bone and jaw relationships. The diagnostic phase guides decisions about extractions, pre-prosthetic procedures, and whether adjunctive support such as implants or root retention is advisable. Once the plan is established, impressions, bite records, and aesthetic selections are taken to communicate precise specifications to the dental laboratory.
The fabrication sequence typically involves try-in appointments to verify tooth position, bite, and facial support so the prosthesis can be refined before final processing. After delivery, adjustments and relines may be needed as the gums and bone remodel, especially following extractions or when immediate dentures are used. Clear communication among the patient, clinical team, and dental technician is essential for predictable, comfortable results.
Wearing new dentures requires an adaptation period during which patients commonly experience increased saliva production, minor soreness, and subtle changes in speech. These reactions are normal and typically improve with practice, such as reading aloud to adapt speech patterns and starting with soft foods while gradually reintroducing chewier items. Small sore spots can usually be relieved with adjustments at follow-up visits, so timely communication with the dental team helps speed the transition.
In the weeks and months after extractions or denture delivery, the gums and underlying bone reshape, which may necessitate relines or minor modifications to restore optimal fit and comfort. Patients should attend scheduled checkups so the prosthesis can be evaluated and adjusted as needed to prevent chronic irritation. With proper follow-up care, most patients achieve stable function and comfortable wear.
Daily denture care preserves the appliance and the health of the supporting tissues: remove and rinse dentures after meals, brush them gently with a soft denture brush or nonabrasive cleanser, and soak them overnight in water or a recommended cleansing solution to keep them hydrated. Cleaning the mouth is equally important; brush remaining natural teeth, gums, tongue, and palate to remove plaque and stimulate circulation. Avoid abrasive household cleaners and hot water, which can damage denture materials and alter fit.
Regular professional checkups allow the dentist to assess tissue health, clean the prosthesis more thoroughly when indicated, and identify early signs of wear or fit changes. If an appliance becomes chipped, cracked, or loose, seek professional repair rather than attempting home fixes. Proper storage and handling reduce the risk of accidental damage and help maintain both hygiene and longevity.
The functional lifespan of a denture varies with material quality, wear patterns, and changes in the mouth, but many patients can expect several years of service before replacement or significant refurbishment is needed. Regular evaluations—typically at least once a year or as recommended by your dentist—help monitor fit, occlusion, and tissue health so relines or repairs can be completed before problems develop. Factors such as bone resorption, systemic health changes, or alterations in bite can accelerate the need for professional attention.
Signs that a denture needs evaluation include persistent soreness, looseness, difficulty chewing, changes in speech, or visible damage to the prosthesis. Timely adjustments can restore comfort and function and may delay full replacement. A proactive maintenance schedule supported by professional care helps preserve oral health and the performance of the prosthesis over time.
Dentures can be integrated into broader restorative plans that include crowns, bridges, implant therapy, and sometimes limited orthodontic treatment, depending on the clinical situation and treatment goals. For example, crowns or root retention can be used to support an overdenture, while implants may be placed to anchor a removable or fixed prosthesis. Coordinating these approaches often improves long-term function, esthetics, and tissue preservation.
Planning combined treatment requires a comprehensive assessment and staged sequencing so each procedure supports the others and maximizes predictable outcomes. The dental team will explain how proposed adjunctive treatments affect timing, recovery, and maintenance to ensure patients understand the pathway to the desired result. Collaborative planning between restorative dentists, surgeons, and laboratory technicians is key to success.
A Plus Dentistry begins with an individualized diagnostic evaluation that considers each patient’s oral health, anatomical features, lifestyle, and long-term goals to recommend the most appropriate denture approach. The treatment process emphasizes precise impressions, aesthetic tooth selection, and try-in visits so the prosthesis matches facial proportions and functional needs. Ongoing communication between the clinical team, the dental laboratory, and the patient helps tailor each step to ensure predictable, comfortable results.
After delivery, the practice provides follow-up care to address fit, function, and maintenance, and discusses options such as overdentures or implant support when additional retention or bone preservation is desired. Patients in Cumming, Georgia, can expect careful planning, modern materials, and a patient-centered approach that focuses on restoring comfort, chewing ability, and a natural appearance. If you have questions about denture options or the process, the team is available to explain choices and next steps.
Quick Links