At the office of A Plus Dentistry, we help patients rebuild healthy, functional smiles after tooth loss. Missing teeth can affect eating, speech, and confidence, and they can set off changes in your bite and jaw that worsen over time. Dental bridges remain a reliable, conservative option for replacing one or more adjacent missing teeth, and this page explains how they work, which situations they suit best, and what to expect from the process.
When a tooth is lost, the immediate visual gap is only part of the story. Without a replacement, neighboring teeth slowly shift toward the empty space. That movement can change how your upper and lower teeth meet, creating a misaligned bite that increases stress on certain teeth and can lead to premature wear or pain in the jaw joints.
Bone health is also affected: the jawbone relies on the stimulation of tooth roots to maintain its volume. Over time, bone in the area of the missing tooth can resorb, changing facial contours and making some replacement options more complicated. Additionally, shifted teeth are harder to clean effectively, which raises the risk of decay and gum disease in surrounding areas.
Beyond the physical changes, a gap in the smile can alter speech and the enjoyment of food. Replacing missing teeth restores not just appearance, but chewing efficiency and articulation, helping patients feel more comfortable in social and everyday situations.
Today’s restorative dentistry emphasizes solutions that look and function like natural teeth. A comprehensive evaluation considers oral health, bone volume, the condition of adjacent teeth, and the patient’s overall goals. From that assessment, we can recommend a plan that balances durability, appearance, and conservation of healthy tooth structure.
Options often include removable partial dentures, traditional fixed bridges that use crowns on neighboring teeth for support, and implant-supported restorations that mimic the missing tooth’s root. Each approach has advantages, and the best choice depends on the specific clinical scenario and long-term goals for oral health.
Materials and digital workflows have advanced greatly, so restorations blend strength with lifelike aesthetics. High-quality ceramics and precision fabrication techniques allow bridges to match color, translucency, and contour, creating a seamless result that integrates with the rest of the smile.
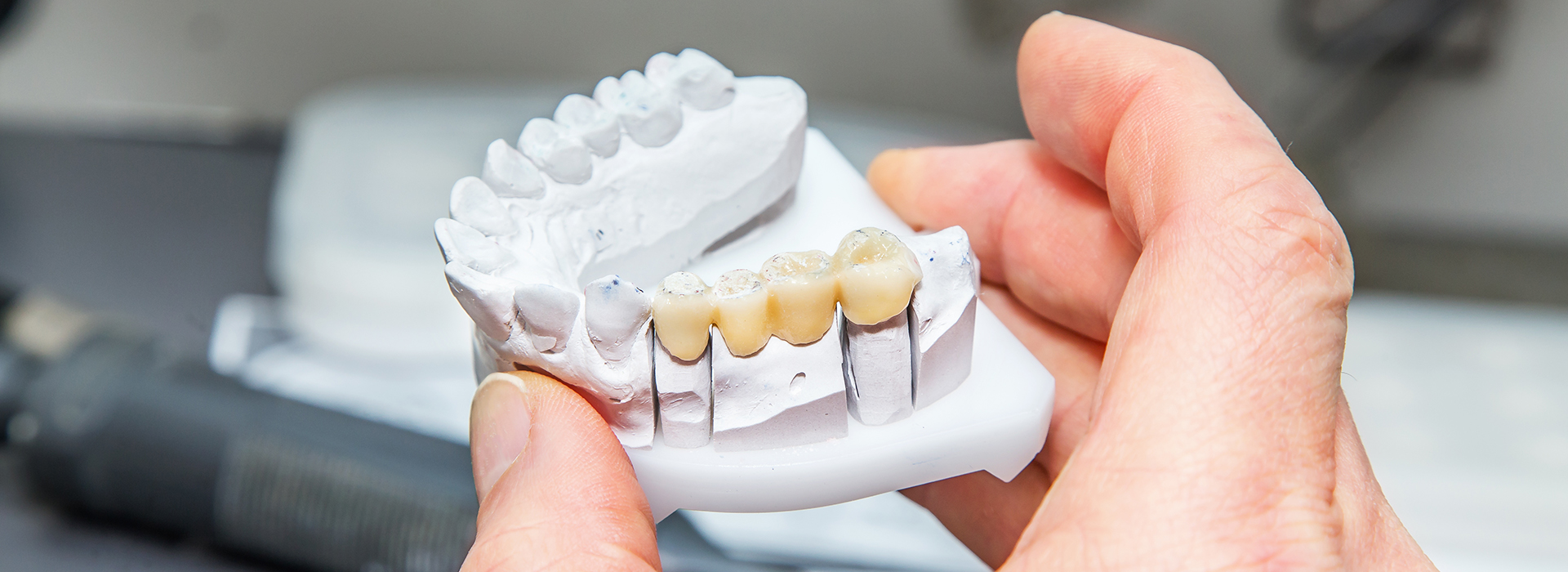
A dental bridge replaces missing teeth with one or more artificial teeth—called pontics—anchored to adjacent supports. In a traditional bridge the supports are natural teeth prepared for crowns; in an implant-supported design, dental implants serve as the anchors. Either way, the bridge spans the gap and restores biting surfaces and alignment.
Structurally, a bridge reestablishes contact points that keep teeth in their intended positions and help distribute chewing forces. This prevents drifting and extrusion of opposing teeth, and it preserves a more stable bite. Properly designed bridges also contribute to speech clarity and efficient chewing, which supports overall oral health.
The look of a modern bridge is often indistinguishable from natural teeth. Porcelain, zirconia, and layered ceramic materials provide excellent strength and optical properties, while careful shade matching and contouring ensure the restoration complements the surrounding dentition.
Several bridge designs are used in practice, each suited to different clinical needs. Traditional fixed bridges rely on crowns placed on the teeth adjacent to the gap; they are a time-tested option when those abutment teeth are healthy or require crowns for other reasons. Cantilever bridges are a variation used when support is available on only one side of the missing tooth, but they require careful case selection because of the directional forces involved.
Maryland (resin-bonded) bridges use a thin framework bonded to the back of adjacent teeth to support a pontic. They are more conservative because they require minimal alteration of neighboring teeth, but they are generally best for small replacements in low-stress areas. Their long-term success can be limited in regions exposed to heavy chewing forces.
Implant-supported bridges are often the most versatile and conservative for preserving adjacent natural teeth. When dental implants replace tooth roots, they provide strong, independent support for pontics without involving neighboring teeth. Implant-supported options also help maintain bone volume because implants transmit chewing forces to the jawbone, stimulating healthy bone maintenance.
Choosing among these designs depends on factors such as the number of missing teeth, health of neighboring teeth and gums, bone availability, and the patient’s functional and aesthetic priorities. A thorough clinical exam and diagnostic imaging guide the decision-making process.
Treatment begins with a comprehensive evaluation that includes a clinical exam, dental imaging, and a discussion of your goals. If gum disease or tooth decay exists, those conditions must be addressed before a bridge is placed. For traditional bridges, the teeth that will act as supports must be strong and healthy enough to receive crowns.
For a traditional bridge, the process generally includes preparing the abutment teeth, taking precise impressions or digital scans, and placing a temporary restoration while the final bridge is crafted. It’s common to experience some sensitivity or mild soreness after tooth preparation; these symptoms typically diminish as the mouth adjusts and the permanent restoration is seated.
When an implant-supported bridge is the chosen route, surgery is required to place the implants. Implant placement is performed with careful planning and is followed by a healing period during which implants integrate with the bone. In some cases a temporary prosthesis can be used to preserve aesthetics while healing occurs; the final bridge is attached once integration is complete and function is confirmed.
After your bridge is cemented or secured, we’ll check fit, bite, and comfort and schedule follow-up visits to monitor adaptation. Good oral hygiene and regular dental care help extend the life of a bridge—brushing, interdental cleaning, and professional checkups are key to maintaining the surrounding teeth and gums.
Dental bridges offer a dependable way to restore missing teeth, protect surrounding structures, and return comfort and confidence to everyday activities. If you’d like to learn whether a bridge is the right solution for your smile, please contact A Plus Dentistry to schedule an evaluation and personalized consultation. We’ll review your options and explain the steps involved so you can make a confident decision about your care.
A dental bridge is a fixed restoration that replaces one or more missing teeth by spanning the gap with artificial teeth called pontics anchored to adjacent supports. Bridges restore the continuity of the dental arch and reestablish contact points that prevent neighboring teeth from drifting. By recovering biting surfaces and alignment, a bridge helps improve chewing efficiency and speech clarity.
Support for a bridge can come from crowns placed on natural abutment teeth or from dental implants that act as independent anchors. The type of support chosen determines how chewing forces are distributed and whether adjacent teeth require alteration. Modern ceramic and zirconia materials provide lifelike color and contour so the restoration integrates with the surrounding dentition.
Good candidates for a dental bridge are people who are missing one or several adjacent teeth and who have healthy or restorable teeth to support a restoration. Candidates should also have healthy gums and sufficient bone support around potential abutment teeth, or be suitable for implant placement if an implant-supported bridge is considered. A thorough clinical exam and diagnostic imaging determine whether a bridge is an appropriate, long-term solution.
Patients with uncontrolled gum disease or extensive decay typically require treatment of those conditions before a bridge is placed. When adjacent teeth are intact and free of large restorations, a traditional bridge may be recommended; when preserving healthy neighboring teeth is a priority, implant-supported or resin-bonded options may be explored. The final recommendation balances oral health, functional needs, and aesthetic goals.
Several common bridge designs are used in restorative dentistry, including traditional fixed bridges that use crowns on neighboring teeth, cantilever bridges that anchor to one side of the gap, and resin-bonded (Maryland) bridges that use a bonded framework attached to the back of adjacent teeth. Implant-supported bridges use dental implants as anchors and are often selected when avoiding alteration of natural teeth is important or when multiple adjacent teeth are missing. Each design has strengths and limitations related to load-bearing capacity, preparation required on neighboring teeth, and long-term stability.
Traditional fixed bridges are time-tested and appropriate when abutment teeth already need crowns or offer solid support. Maryland bridges are more conservative but work best for small replacements in low-stress areas. Implant-supported bridges help preserve bone and provide independent support, making them a preferred option when sufficient bone is available and implant surgery is acceptable.
An implant-supported bridge is anchored to dental implants that replace tooth roots, while a traditional bridge relies on crowns cemented to prepared natural teeth adjacent to the gap. Because implants transmit chewing forces to the jawbone, they help preserve bone volume and avoid altering neighboring healthy teeth. Implant-supported bridges can be particularly advantageous when multiple adjacent teeth are missing and preserving natural tooth structure is a priority.
Traditional bridges are generally completed without surgery and can be faster to place when abutment teeth are already suitable, but they require reduction of adjacent teeth to accept crowns. Implant-supported restorations require surgical placement and a healing period for osseointegration before the final restoration is attached. The ideal choice depends on oral health, bone availability, patient preferences, and long-term maintenance considerations.
The evaluation begins with a comprehensive clinical exam and diagnostic imaging to assess the condition of adjacent teeth, gum health, and underlying bone. Your dentist will review medical and dental history, discuss functional and aesthetic goals, and explain suitable restorative options based on the findings. At the office of A Plus Dentistry, this planning stage also includes reviewing digital scans or impressions and outlining the anticipated sequence of treatments so patients understand each step.
If periodontal disease or decay is present, those issues must be addressed before placing a bridge to ensure a stable foundation. For implant-supported options, additional imaging such as CBCT may be used to evaluate bone quantity and plan implant positions. The treatment plan will identify whether a temporary restoration is needed and establish follow-up visits to verify fit and function after placement.
The process for a traditional fixed bridge usually begins with preparing the abutment teeth by removing a portion of enamel to create room for crowns. After preparation, precise impressions or digital scans are taken and a temporary bridge is placed to protect the prepared teeth while the laboratory fabricates the final restoration. Once the permanent bridge is ready, the dentist checks fit, shade, and bite before cementing the restoration in place.
Patients commonly experience mild sensitivity or soreness following tooth preparation, and these symptoms typically resolve as the mouth adjusts. The dentist will verify occlusion and make any minor adjustments needed to ensure comfort and efficient chewing. Regular follow-up visits allow the clinician to monitor the bridge and surrounding tissues over time.
Daily oral hygiene is essential for the longevity of a dental bridge and the health of supporting teeth and gums. Brush twice daily with a fluoride toothpaste and use interdental cleaning aids, such as floss threaders, super floss, or interdental brushes, to clean beneath pontics and around abutments. Maintaining regular professional cleanings and dental exams helps detect early issues like decay at margins or gum inflammation.
Avoiding habits that place excessive force on the restoration, such as chewing ice or using teeth to open packages, reduces the risk of fracture or loosening. If you grind or clench your teeth, discuss protective options like a night guard to protect both the bridge and natural dentition. Promptly report any looseness, sensitivity, or changes in bite so the dentist can intervene before more significant problems develop.
Potential complications include decay on abutment teeth, gum disease around supporting structures, loosening or debonding of the bridge, and fracture of pontics or crown material. Because traditional bridges require preparing adjacent teeth, those teeth may become more susceptible to sensitivity or future restorative needs if not properly maintained. Resin-bonded designs may have higher risk of debonding in high-stress areas, while implant-supported bridges carry surgical risks such as infection or implant failure in rare cases.
Early detection and management of complications rely on regular dental visits and meticulous home care. Addressing periodontal issues, treating decay promptly, and ensuring proper fit and occlusion reduce the likelihood of long-term problems. Your dentist will explain which risks apply to your specific case and outline preventive steps to protect the restoration and surrounding tissues.
The lifespan of a dental bridge varies with factors such as the type of bridge, the quality of oral hygiene, the health of supporting teeth and gums, and the materials used. With consistent care and routine dental maintenance, many bridges remain functional for several years and often a decade or more; individual results depend on wear, oral environment, and habits like grinding. Regular checkups allow the dental team to identify wear or changes early and to recommend maintenance or replacement when appropriate.
Failures commonly occur because of recurrent decay on abutment teeth, gum disease, or mechanical complications such as fracture or loosening. Good home care, professional cleanings, and addressing parafunctional habits help extend the restoration’s service life. When replacement becomes necessary, your dentist will review options that preserve oral health and restore function.
Choosing among a bridge, implant, or removable partial denture involves assessing oral and general health, the condition of adjacent teeth, bone availability, aesthetic goals, and functional priorities. Implants preserve bone and often avoid altering neighboring teeth, while traditional bridges can be an effective solution when nearby teeth already require crowns. Removable partial dentures are a less invasive option for certain cases and may be appropriate when restoring multiple nonadjacent teeth or when an interim solution is needed.
We recommend a personalized consultation to review diagnostic imaging and discuss the benefits and trade-offs of each approach based on your situation. The clinical exam and patient goals guide a recommendation that balances durability, preservation of natural tooth structure, and expected maintenance. To explore which option fits your needs, contact the office of A Plus Dentistry in Cumming, Georgia for a detailed evaluation and treatment discussion.
Quick Links